Two medical specialists say physical therapy needed for man allegedly isolated in group home
John Davidson, a man with an intellectual disability, is declining physically in his group home and has not received needed physical therapy there after an extended stay last year at Tewksbury State Hospital, according to two medical specialists.
One of the physicians, Adam Harris, a specialist in spinal disorders at New England Baptist Hospital, on Wednesday (February 16) recommended an eight-week regimen of physical therapy for John at Spaulding Wellesley rehabilitation center.
In a summary of an examination of John on Wednesday, Dr. Harris wrote that John had “deconditioned” after his stay at Tewksbury. Harris’s summary stated that following that hospitalization, John was “never transferred to outpatient therapy.”
A second specialist, Steven Cohen, a gastroenterologist with Beth Israel Deaconess Medical Center, wrote in a medical progress note, dated February 3, that John was declining physically due to a lack of physical therapy and other stimulative activities.
John has been confined to a wheelchair following the stay at Tewksbury, which reportedly stemmed from a broken leg that he suffered from a fall outside his group home in 2019.
The two medical assessments corroborate a contention by John’s mother, Christine Davidson, that John has not been provided with stimulative activities at the residence, which is operated by WCI, Inc., a corporate provider to the Department of Developmental Services (DDS). She said he was not receiving physical therapy and has had no functioning day program. She also said he is depressed and wants to be allowed to visit her at her home.
Cohen also wrote in the progress note that he believes John should be living with his mother rather than in the group home.
“Overall, I’m very concerned about prognosis due to poor conditioning,” Cohen’s progress note stated. “Aggressive PT is best hope. Would be best served if living with his mother whose excellent care I have witnessed for over 20 years.”
Cohen added that, “John is terribly deconditioned and needs PT and aquatherapy.”
Cohen also stated that John was “clearly deteriorating” in terms of his mobility, and was “too weak” to be safely examined on a table in Cohen’s office. He further wrote that John was “upset over not being home.”
Breathing mask unhygienic
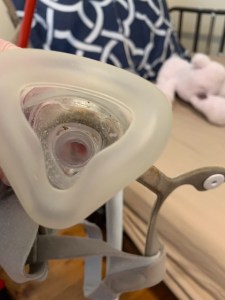
In addition to his concerns over John’s physical condition, Cohen stated in his February 3 progress note that a breathing mask that is apparently being used on John at the group home to treat sleep apnea was “apparently not hygienic.” Christine sent us the photographs below that her partner, Carmine Tocco, took on February 2 of John’s breathing mask, which is attached to a Bi-PAP machine at the WCI residence.
Christine Davidson said she has spoken to the group home staff about the breathing mask and about what she said were other poor hygienic conditions in the residence.
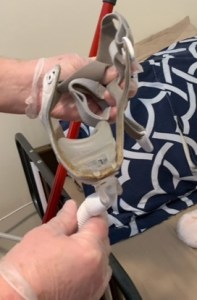
Photographs taken February 2 of a reportedly dirty breathing mask apparently being used on John in his group home.
Questionable abuse charge appealed
In a recent blog post, we reported that we have raised numerous questions about the accuracy of a report written by the Disabled Persons Protection Commission (DPPC), which concluded last October that Christine abused John after she gave him an “undetermined” amount of cough syrup and Tylenol last June. Since then, John has been subject to a prohibition on visits home.
Christine’s attorney, Thomas Frain, who is also COFAR’s president, filed an appeal with DPPC of the abuse finding. The appeal notes that the cough syrup and Tylenol that Christine provided her son had been prescribed by his primary care doctor, and that there was no evidence presented by the DPPC that Christine did not follow the prescriptions.
Christine is a co-guardian of her son. The other co-guardian, George Papastrat, is Christine’s nephew and lives in North Carolina. Under the co-guardianship agreement, Papastrat has the authority to make medical and other decisions about John’s care. Papastrat has not responded to emails I have sent him raising concerns about John’s care.
Numerous medical issues
John has Down Syndrome, “multiple gastrointestinal issues,” Celiac disease, obesity, severe osteoporosis, and several other medical conditions. He is also continuing to experience pain from the leg fracture in 2019.
In addition to the lack of physical therapy, Cohen said John was not being taken out of the residence for aquatherapy, an activity he previously enjoyed.
DPPC placed blame on mother regarding breathing mask
In accusing Christine in October of abuse, the DPPC alleged that in addition to giving him an “undetermined amount of cough syrup and Tylenol,” she had failed to provide prescribed breathing therapy support “causing (John) to lose consciousness” in the morning of June 21. The prescribed therapy was the use of the breathing mask and Bi-PAP breathing assistance machine at night.
Christine was unable to wake John up in the morning of June 21, and called 911. John was brought to the Newton Wellesley Hospital ER. He quickly recovered after being given oxygen.
Christine maintains that the Bi-PAP machine and mask were not delivered to her until June 22, the day after John’s episode of hypoxemia or low oxygen level. She also said she did not receive necessary training in how to use the machine. When she inquired of a group home staff member about receiving training, she said she was told there would be no opportunity for that.
Christine said the breathing machine was later removed from her home by a group home staff member, and that she later saw the machine’s breathing mask on the floor of John’s room and noticed that it looked dirty. She said when she brought that to the attention of the staff, they did not respond to her.
Following the DPPC’s decsion to level the abuse charge against Christine, DDS issued an “action plan” in October that recommended sharply curtailing contact between Christine and John. The DDS action plan also stated that the Bi-PAP machine “should be operated by trained residential staff.”
Attempts to contact DDS commissioner and other officials
On February 14, I sent an email to DDS Commissioner Jane Ryder, asking whether she would inform either us or Christine of what measures, if any, DDS may be taking to address the concerns raised by Dr. Cohen and Christine about John’s care.
I sent a similar email the same day to Nancy Silver Hargreaves, president and CEO of WCI. To date, I haven’t received a response from either Ryder or Hargreaves.
On January 10, I wrote to Gail Gillespie, DDS Metro Region director, and Joan Thompson, DDS area director, about John’s situation. I have not received a response from Gillespie.
On January 11, Thompson responded with a two-sentence email stating that I would need written authorization from both co-guardians in order for her to release any information about the matter.
As we have previously stated, we think DDS should conduct an investigation of the conditions under which John is living, and should take immediate steps to provide him with physical therapy and other activities – particularly those activities recommended by Drs. Cohen and Harris.
We have also urged DDS to take both John’s and Christine’s often-stated wishes into account and begin by arranging for visits home for John. We concur with the assessment that the best hope for John is to return home to live with his mother.
DDS appears to be using a disagreement between co-guardians; one, John’s mother who lives nearby and has taken care of him his whole life, and the other, a nephew who is uninvolved and lives out of state, as an excuse to not provide information on this ongoing travesty. As John continues to deteriorate, how does DDS and its provider agency excuse their lack of concern, especially in light of medical recommendations from John’s own physicians? This is not the DDS I used to know. Where is the empathy and concern for John and his mother? Where is the concern for his physical and mental wellbeing? John should be evaluated at an ICF (Hogan or Wrentham) to assess his medical condition before it is too late. I feel certain that the co-guardian would agree to have John assessed if DDS recommended it. Is John going to deteriorate physically and mentally and die at this group home before something is done?
LikeLiked by 1 person
Just an aside, running a group home for clients with complex needs and staff shortages, including nursing support, I have to give praise for all the caregivers and house managers that try so hard to do.an impossible job. I have been in direct care and manager of a home and I gave it all I had, yet still.things were far from perfect. I remember I used to say to coworkers I felt like I was working in the emergency department. And this reflection is about a good group home with good support systems.
LikeLiked by 1 person
My heart goes out to Christine and John! I went through basically the same situation with my brother , Tom Kosak, in the western part of this state. Their charges of abuse on Christine are to stop her(the same happened to me). FYI if Tom Frain could get John into Wrentham Developmental Ctr for re-habilitation, they have an indoor pool on grounds/although with the Covid aspect, I m not sure how that would go. God bless her to keep fighting them for him
LikeLiked by 1 person
While the particulars are horrendous if parents and guardians prepare Person Centered Service Plans that are more specific and descriptive of the over goals it will begin to establish the need for specific programs that are not ignored. There are some key areas that a Person Centered Service Plan can address such as the need for Daily Structure that and ICF or Workshops or Day services program can provide. I will leave it to others who are far more gifted writing expansive and descriptive Person Centered Service Plans. Thomas Spellman
LikeLiked by 1 person
This story is heartbreaking. I wonder if Christine is aware of the wonderful care John could receive at Wrentham Developmental Center? His needs could readily be met by on-site PTs and OTs and there is a wonderful indoor pool with appropriate activities. He would not be isolated as each residence at WDC provides a range of activities and promotes community among the residents. Medical care is excellent, and John could continue with Dr. Cohen as well as any other specialists he may need. His mother and her partner would be welcomed as integral to John’s care. When I read this, and other instances, of family and group residences staff being at odds, it is so troubling. I truly hope a suitable, safe and kind plan can be made with John as the focus…and with his family supported and included. Stop the blaming, finger pointing and lack of transparency…
LikeLiked by 1 person