Advocacy continues following Senate budget decision on Wrentham and Hogan amendments
Our two budget amendments aimed at preserving the Wrentham and Hogan Intermediate Care Facilities (ICFs) for adults with intellectual and developmental disabilities ultimately did not move forward in the Massachusetts state Senate during its debate last month on the Fiscal Year 2027 state budget.
This outcome was not unique; out of the 1,158 amendments filed to the Senate budget, more than half were either withdrawn or rejected. Senate Ways and Means Committee Chair Michael Rodrigues previously indicated that “there is not a ton of room for amendments” this budget cycle.
The amendments, 411 and 555, filed by Senate Minority Leader Bruce Tarr and Senator Becca Rausch, would have altogether affirmed a right to care at Wrentham and Hogan for persons found to be eligible for ICF-level care, required the Department of Developmental Services (DDS) to report on its efforts to offer these settings as a choice for residential care, and protected current ICF residents from involuntary discharge.
In both the House and Senate, the adoption of budget amendments are subject to decisions by the legislative leadership. Most amendments are voted on in bundles, and only a limited number are formally considered by the full chamber. As a result, our amendments were not individually debated or voted on in either chamber.
Our budget language was consistent with federal law and aligned with DDS’ movement toward “self-direction,” which expands the role of individuals and families in the planning and selecting of services.
The Senate results follow our amendment effort in the House. There Representative Marcus Vaughn filed three amendments containing our language. Although the amendments received the bipartisan support of 19 legislative co-sponsors, they also were not adopted.
Because our amendments did not advance in the House or Senate, our language will not be incorporated into the FY ‘27 state budget. However, we are hopeful that we have laid the groundwork for the reintroduction of our proposed language next year to save the Wrentham and Hogan facilities.
We are pleased that during this year’s budget debates, nearly a quarter of the Senate formally engaged on this issue by either sponsoring or co-sponsoring the amendments. It is encouraging to know that we are spreading awareness across the legislature, which oversees state agencies such as DDS. As noted, we believe this sets the groundwork for future legislative advocacy efforts.
This year marked our first sustained attempt to modify the state budget language.
Senate amendment co-sponsors
We would like to thank Senate Minority Leader Bruce E. Tarr (R, First Essex and Middlesex) and Senator Rebecca L. Rausch (D, Norfolk, Worcester and Middlesex), the principal sponsors of our amendments, along with the following co-sponsors:
Senator Pavel M. Payano, D, First Essex
Senator Jason M. Lewis, D, Fifth Middlesex
Senator John F. Keenan, D, Norfolk and Plymouth
Senator James B. Eldridge, D, Middlesex and Worcester
Senator Nick Collins, D, First Suffolk
Senator William J. Driscoll, Jr., D, Norfolk, Plymouth, and Bristol
Senator Vanna Howard, D, First Middlesex
COFAR member outreach
We additionally would like to thank our COFAR members for their tireless advocacy. Whether emailing or calling their state senators, sharing our posts on social media, or encouraging others to contact their legislators, we were heartened by the outpouring of support. Your help was essential to the progress that we were able to achieve this year. Thank you for sharing your stories and perspective.
Future legislative advocacy efforts
We will work to enact this language again next year since we believe the facilities are in danger of closure.
The Wrentham and Hogan centers offer a high level of federally regulated care for individuals with some of the most profound disabilities. They also provide more than 1,000 jobs for direct care workers, clinicians, medical personnel, and others, according to the latest data available from DDS.
The population at both facilities has decreased significantly, however. Families report that they are not informed of ICF options or have their placement requests rejected. If these trends continue, closure of these facilities is inevitable.
It was only last year that Governor Maura Healey announced the proposed closure of Pappas Rehabilitation Hospital for Children, a state-run residential hospital for children with disabilities that is reportedly now experiencing similar restrictions on admissions. We remain committed to safeguarding essential state-operated services for people with disabilities amid rampant privatization.
We encourage you to continue sharing your perspective with legislators to keep attention on this issue. If you are interested in participating in future legislative advocacy efforts, please contact us at info@cofar.org. Together we can preserve the Wrentham and Hogan centers.
We are seeking co-sponsors in the Senate of our amendments to save the Wrentham and Hogan centers
Our fight to preserve the Wrentham and Hogan Intermediate Care centers has now shifted to the state Senate, where two budget amendments to save the centers have been filed in anticipation of next week’s budget debate in the upper chamber.
We are urging the senators to co-sponsor budget amendments 411 and 555, which would affirm a right to residential placements at Wrentham and Hogan.
The two facilities, which are in danger of closure, offer a high level of federally regulated care and provide more than 1,000 jobs for direct care workers, clinicians, medical personnel, and others, according to the latest data available from the Department of Developmental Services (DDS).
The amendments, which have been filed by Senate Minority Leader Bruce Tarr and Senator Rebecca Rausch, would affirm a right to care at Wrentham and Hogan for persons found to be eligible for ICF-level care, and would require DDS to report on its efforts to offer these settings as a choice for residential care.
These amendments are not only consistent with federal law, but also align with the Commonwealth’s policy of encouraging “self-direction” — ensuring that individuals and families have a meaningful role in planning and choosing services.
Nevertheless, DDS has routinely denied requests for placements in the facilities, implying that clients of the Department do not have a right to such placements. As a result, the census in both facilities has continued to drop, and we believe the centers are on a path to closure due to attrition.
Preserving the Wrentham and Hogan Centers is also part of a broader effort to protect essential state-operated services, including the Pappas Rehabilitation Hospital. Each of these facilities faces an increasing risk of closure due to ongoing restrictions on admissions.
During the budget debate in the House last month, our amendments received the bipartisan support of 20 legislators, with 13 Democratic and 6 Republican co-sponsors. Unfortunately, the language in our amendments was not included in the final consolidated amendment in the House.
We are hoping for a better outcome in the Senate for this critically important effort to preserve these facilities. Please contact your state senator and ask them to co-sponsor budget amendments 411 and 555. You can find your senator here. Thanks!
House leadership rejects the right to care at Wrentham and Hogan Centers
Under the state Legislature’s less-than-fully-democratic state budget process, our budget amendments to preserve the Wrentham and Hogan Intermediate Care Facilities (ICFs) were rejected last week in the House of Representatives without either a vote or debate on any of them.
It was frustrating because our amendments had garnered bipartisan support before each was stripped of its language by the House leadership. There were 18 cosponsors of our primary amendment, including 12 Democrats and 6 Republicans. There were 16 cosponsors of each of two other amendments that had been filed on our behalf.
The good news is the battle to preserve the ICFs now shifts to the state Senate, which is scheduled to debate its version of the Fiscal Year 2027 state budget starting the week of May 18. The bad news is, it might be difficult to find a senator to file our primary amendment, which would affirm a federally sanctioned right to residential placements in ICFs such as Wrentham and Hogan.
Last week, the leadership in the House assigned our amendments to a large “consolidated amendment,” which included dozens of amendments involving “public health and mental health and disability services.” However, the leadership then stripped the language in our amendments from the consolidated amendment.
Under the consolidated budget amendment process in the House, the House leadership places the vast majority of the thousands of individual amendments filed by House members each year in a small number of consolidated amendments. The leadership then decides what language from those individual amendments it wants to preserve, and allows up or down votes on the consolidated measures. Those consolidated amendments are always approved.
While individual legislators can lobby the leadership for approval of their amendments, it is ultimately the leadership’s decision whether to allow individual votes on the amendments or simply strip the language from them.
Our primary amendment, which had been filed Representative Marcus Vaughn, would ensure a choice and right to ICF care for those who have been found to be eligible for it. That amendment and our two related amendments were filed on our behalf by Vaughn, whose district includes Wrentham.
Among the cosponsors of each of the amendments were House Minority Leader Bradley Jones; and Democratic Representatives Lisa Field, a member of the Mass. Nurses Association, and Sally Kerans, who represents the Town of Danvers in which the Hogan Regional Center is located.
We think the reason our amendments were rejected has to do with the likely opposition to them by the Department of Developmental Services (DDS). As we have reported, the administration rarely allows admissions to either Wrentham or Hogan, and has been allowing those facilities to die by attrition. Yet these facilities are Medicaid certified centers that provide residential care, which the late federal District Court Judge Joseph Tauro described as “second to none anywhere in the world.”
While it seems unlikely that we will gain passage this year of our budget language asserting a right to ICF care – at least partly due to the lack of true democracy in the legislative process – our longer-term hope is to lay the groundwork for passage of the language next year. But time is running out for Wrentham and Hogan, given that their residential populations, or census, have been steadily declining.
We are urging our members to email their state senators as soon as possible, and ask them to agree to file an amendment to establish a right to ICF care for those who are eligible for that level of care. We will follow up with every senator who expresses a willingness to file such an amendment.
You can find your state senator here.
In sum, it is a troubling statement about the Massachusetts legislative process that a small number of legislative leaders can foreclose the opportunity for separate votes and debate on measures that have significant support in the chambers. It reduces the input of the rank and file membership of the Legislature, and, even more importantly, of the public whom those legislators represent.
In our amendments, we are not seeking more funding for programs — we are seeking just the affirmation of a common sense right that is already established in federal law. We hope the Legislature will ultimately support that right, and the administration will finally see the matter in that light as well.
Cosponsors in the house of our amendments
We would like to thank Representative Marcus Vaughn, the principal sponsor of our amendments, and the following cosponsors in the House of our primary amendment, and, in most cases, our additional amendments. They are Representatives:
Bradley H. Jones, Jr. R, Reading, House minority leader
Lisa Field, D, Taunton
John J. Marsi, R, Worcester
Sally P. Kerans, D, Danvers
David T. Vieira, R, Bourne
Lindsay N. Sabadosa, D, Northampton
Michael J. Soter R, Uxbridge
Natalie M. Higgins, D, Leominster
Amy Mah Sangiolo, D, Newton
James K. Hawkins, D, Attleboro
Norman J. Orrall, R, Berkley
Kate Donaghue, D, Northboro
Adam J. Scanlon, D, North Attleboro
David Allen Robertson, D, Tewksbury
Michael S. Chaisson, R, Foxboro
Paul McMurtry, D, Dedham
Greg Schwartz, D, Newton
David Henry Argosky LeBoeuf, D, Worcester
An additional House member, Representative Simon Cataldo, D, Carlisle, cosponsored one of our amendments, which would require DDS to report to the Legislature on steps taken to inform families of choices for care, including ICF residential care.
Bipartisan support grows for our budget amendments to save Wrentham and Hogan Centers
As the state House of Representatives begins debate today on the Fiscal Year 2027 state budget, we are gaining bipartisan support for our proposed amendments asserting a right of persons with intellectual and developmental disabilities (I/DD) to placements at the Wrentham and Hogan Intermediate Care Facilities (ICFs).
This is a right that not only aligns with federal law, but is consistent with the state’s policy of encouraging “self-direction” among clients in planning and choosing their services.
When it comes to Wrentham and Hogan, not only does the Department of Developmental Services (DDS) not inform disabled individuals and their families of the existence of those facilities, but the Department implies they don’t have a right to placements there.
Wrentham and Hogan are the last two remaining ICFs for persons with I/DD in Massachusetts, and we are concerned that the centers are heading toward closure.
As of today, 12 legislators have indicated their support for Amendment 695, which states that people with I/DD, who have been found to be eligible for ICF-level care, have a right to placement in an ICF residential setting.
A second amendment, which has also gathered the same cosponsors (Amendment 699), requires DDS to report on its efforts to inform families of all residential choices available for care, including ICF care. And a third amendment (Amendment 703) states that residents of ICFs cannot be involuntarily discharged from those facilities.
The cosponsors so far consist of six Democrats and six Republicans, including Republican Representative Marcus Vaughn, the principal sponsor of each of the amendments. Vaughn represents a district that includes the Wrentham Developmental Center.
Among the cosponsors are:
Representative Bradley Jones, a Republican from North Reading, and the House minority leader
Representative Lisa Field, a Democrat from Taunton, who is also a member of the Mass. Nurses Association. The MNA is supporting the effort to keep Wrentham and Hogan open
Representative Sally Kerans, a Democrat from Danvers, in which the Hogan Regional Center is located
Representative John Marsi, a Republican from Worcester
Representative Lindsay Sabasdosa, a Democrat from Northampton
Representative David Viera, a Republican from Bourne
Representative Michael Soter, a Republican from Bellingham
Representative Natalie Higgins, a Democrat from Leominster
Representative Amy Mah Sangiolo, a Democrat from Newton
Representative James Hawkins, a Democrat from Attleboro
Representative Norman Orrall, a Republican from Lakeville
We would urge all 160 House members to support these amendments because the language in them stakes out a commonsense position in favor of individual choice. We have always advocated for a full continuum of care for the most vulnerable citizens among us.
As advocates of the Wrentham and Hogan Centers have long pointed out, one size does not fit all. Community-based group homes can be the best choice for many, if not most, people with I/DD. But for a segment of that population, the community system is either not desired or it cannot meet their complex needs.
There can be no clearer example of that than the case of Kristen Robinson, who has been denied admission to Wrentham even though she is legally blind, quadriplegic, and has profound ID and complex medical issues. No community-based residence or nursing home could or would provide residential care for her.
Kristen was finally admitted to Hogan, after a months-long battle by her family, where she is now thriving.
But Kristen is the exception. Potentially, thousands of persons are waiting in Massachusetts for residential placements, and neither Wrentham nor Hogan is being offered as an option to them.
Questionable claim of cost savings
A series of administrations has long argued that closing congregate care facilities and placing residents in group homes saves money. But this argument is short-sighted and misleading.
As a recent report by our partner organization, the Saving Wrentham and Hogan Alliance, has shown, comparisons of the cost per resident of group home and ICF residents are comparisons of apples to oranges. ICF costs are reflected in the ICF line item in the state budget each year. Those include staffing costs, clinical care, food, housing, and facility costs.
In contrast, the costs of serving people in group homes show up in several state and federal budgets, including MassHealth, Housing and Urban Development (HUD) subsidies and in SNAP benefits, in addition to the DDS community residential line item.
The Saving Wrentham and Hogan Alliance report makes the overall point that the community-based group home system incurs an estimated $1.3 billion in taxpayer costs each year that are not included in the overall $3.3 billion DDS budget.
The DDS line item for corporate group home providers has doubled from a decade ago to more than $2 billion in the current fiscal year. During that same period, the line item for the Wrentham and Hogan facilities has declined by about 14% to roughly $130 million.
So where is the savings in closing ICFs and placing people in the group home system?
Right to an ICF
The assertion in Amendment 695 that ICF-eligible individuals in Massachusetts have a right to placement in an ICF aligns with the establishment of that right in the federal Medicaid Law and regulations.
The landmark Boulet v. Cellucci federal court decision (107 F. Supp. 2d 61 (D. Mass. 2000) cites the Medicaid statute (42 U.S.C., § 1396a(a) (8)), and explicitly states, “…to the extent that the plaintiffs have requested ICF/MR (now ICF/IDD) services, the state must provide those services reasonably promptly.”
The Boulet decision, which was written by U.S. District Court Judge Douglas Woodlock, required DDS to provide residential services promptly to thousands of clients who had been waiting for placements, in some cases for years. Unfortunately, the decision hasn’t led to a resolution of the problem. Not only are people still waiting months or years for placements, but DDS is badly underutilizing its state-run residential resources, which could help mitigate the problem.
DDS’s policy of personal choice
The right to choose an ICF also aligns with DDS’s stated policy that individuals and their guardians should be able to “self-direct” their care. The DDS’s Self-Directed Services website page contains the following statement:
DDS helps an individual to have more control in their life and to make decisions about services based on their vision, path, preferences, beliefs and abilities. The individual decides who helps them and how they want that help to be provided, based on what they want in life and their personal goals.
Placement in an ICF should be a part of that choice.
Connection to fight to preserve Pappas
Finally, we believe there are a number of parallels between the Healey administration’s reported policy of restricting admissions to the Pappas Rehabilitation Hospital and its policy of denying most requests for placement at Wrentham and Hogan.
In sum, our budget amendments are intended to preserve choice and to ensure respect for the wishes and preferences of DDS clients and their families. We hope all 160 House members would agree that the right to a choice of residential options along the entire spectrum of care should be respected and upheld.
Please continue to call or email your House member and ask them to cosponsor or sign onto Amendments 695, 699, and 703. You can find your legislator here. Thanks!
Our proposed budget amendments assert a right to placement in an ICF in line with the landmark federal Boulet case
As the Massachusetts House of Representatives gets ready to debate the Fiscal Year 2027 state budget next week, we are advocating for three budget amendments to help ensure the preservation of the Wrentham and Hogan Intermediate Care Facilities.
At our request, Representative Marcus Vaughn, whose district houses the Wrentham Center, has filed Amendment 695 to the budget legislation. This amendment states that people with intellectual and developmental disabilities (I/DD), who have been found to be eligible for ICF-level care, have a right to an ICF residential setting.
A second amendment filed by Rep. Vaughn (Amendment 699) requires DDS to report on its efforts to inform families of all residential choices available for care, including ICF care. And a third amendment (Amendment 703) states that residents of ICFs cannot be involuntarily discharged from those facilities.
Among the House members who have told us they support the proposed amendments and will co-sponsor them are Reps. Lisa Field, a member of the Mass. Nurses Association; Lindsay Sabadosa, and Joseph McKenna. We are urging our members to call or email their House member and ask them to cosponsor or sign onto Amendments 695, 699, and 703. You can find your legislator here.
DDS failing to recognize the right to ICF care
The Department of Developmental Services (DDS), which operates the Wrentham and Hogan Centers, has routinely denied requests for placements in those facilities, implying that clients of the Department do not have a right to such placements.
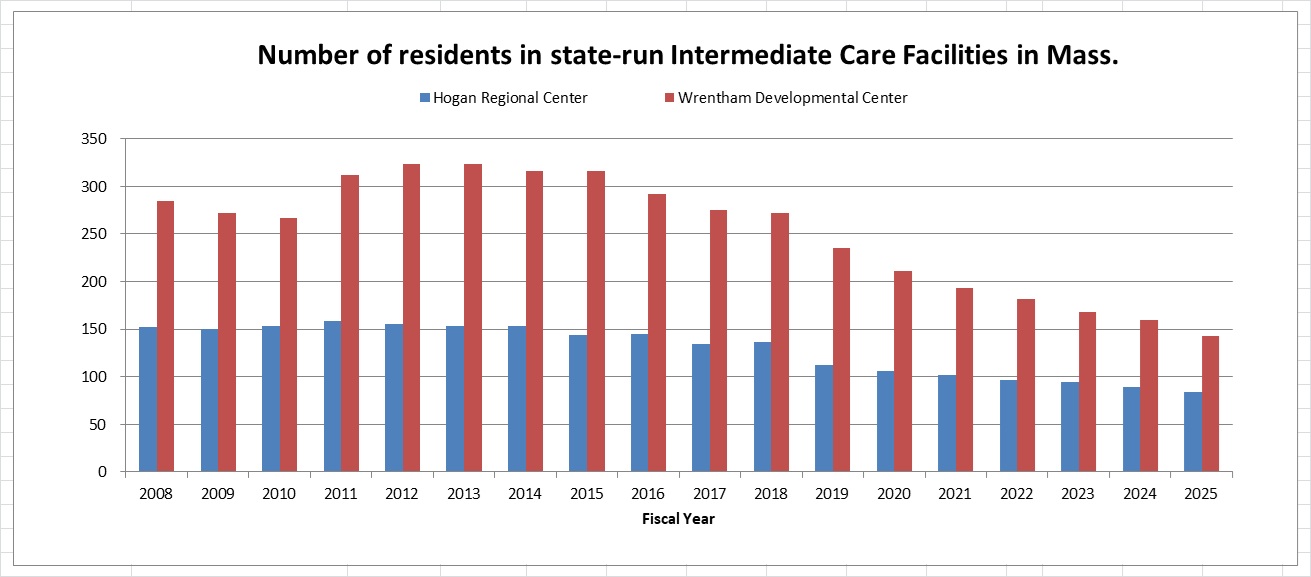
At the same time, DDS has not provided clear or acceptable criteria for admission to Wrentham or Hogan. As a result, the census in both facilities has continued to drop, and we believe the centers are on a path to closure due to attrition. (See the graph below.)
In at least two cases in recent years in which family members have filed administrative appeals to gain admission to Wrentham, a DDS hearing officer accepted the Department’s argument that the federal Medicaid law “does not entitle (the individual) admission to an Intermediate Care Facility…”
DDS’s only stated criterion for admission to Wrentham in those appeals was: “DDS avoids institutionalization at the ICFs except in cases where there is a health or safety risk to the individual or others, and generally, when all other community-based options have been exhausted.”
Wrentham and Hogan are the only two congregate-care ICFs remaining in Massachusetts. They are state-run, federally regulated, and Medicaid-certified. They provide specialized services for people with profound disabilities, including 24/7 medical care and structured educational, vocational, and recreational programming.
The loss of these centers would mean the loss of critical care for individuals with the most profound disabilities. Given that thousands of people are reportedly waiting for residential placements in the DDS system, individuals are already facing increased hospitalizations and emergency room visits, and many families are forced to take on care beyond their capacity. The loss of Wrentham and Hogan would only worsen this situation.
Boulet case confirms a right to ICF care under federal law
In our view, eligible DDS clients do have a right to choose care in an ICF. That right is established in the federal Medicaid law and regulations, and is affirmed in the landmark Boulet v. Cellucci federal court decision (107 F. Supp. 2d 61 (D. Mass. 2000).
The Boulet decision, which was written by U.S. District Court Judge Douglas Woodlock, required DDS to provide residential services promptly to thousands of clients who had been waiting for placements, in some cases for years.
Woodlock’s decision states that there is a right to ICF care, provided with “reasonable promptness,” for those clients who are found to be eligible for that level of care and request it. The decision cites and closely tracks the federal Medicaid statute and regulatory language that we have been citing for some time.
- The Boulet decision states that if a state includes ICF services in its state plan, which Massachusetts does, the Medicaid law requires “that this type of ‘medical assistance’ be provided ‘with reasonable promptness.'” The decision then cites the Medicaid statute (42 U.S.C., § 1396a(a) (8)), and adds, “Therefore, to the extent that the plaintiffs have requested ICF/MR (now ICF/IDD) services, the state must provide those services reasonably promptly.”
- The decision also discusses the Home and Community Based Services (HCBS) waiver, and states that under the waiver, an ICF-eligible individual or his legal representative “will be: 1. informed of any feasible alternatives under the waiver; and 2. Given the choice of either institutional or home and community-based services.” The decision further cites the Medicaid regulation, 42 C.F.R. § 441.302(d), as explicitly requiring the choice of either institutional or HCBS care.
Woodlock’s decision also cites a 1998 11th Circuit U.S. Court of Appeals decision (Doe v. Chiles,136 F.3d 709 (1998) at 721) that held that states cannot justify long delays for covered services, including those provided by ICFs/IDD.
We think our proposed budget amendment is therefore consistent with the holdings of both federal law and with Boulet, both of which recognize that eligible clients must be informed of all feasible residential alternatives and given a choice among service settings, including ICF care.
We believe that asserting a right in state law to ICF care for eligible individuals will make it clear that DDS cannot deny admissions for Wrentham or Hogan without establishing clear criteria for admissions that include factors such as the degree of a person’s cognitive impairment.
That should ensure that the doors to those facilities are reopened to eligible clients who seek placements there, and thereby ensure the preservation of those critically important centers.
The Wrentham and Hogan Centers should be on the preservation list along with the Pappas Rehab Hospital
We are supporting the efforts of a number of unions and other advocates for the disabled to save the Pappas Rehabilitation Hospital from closure.
We are also pushing, at the same time, to add the state’s two remaining Intermediate Care Facilities for persons with intellectual and developmental disabilities (ICF/IDDs) — the Wrentham Developmental Center and the Hogan Regional Center — to the list of endangered facilities that must be preserved in Massachusetts.
There appear to be a number of parallels between the Healey administration’s reported policy of restricting admissions to the Pappas Hospital, and its policy of denying most requests for placement at Wrentham and Hogan.
The administration has placed “overly restrictive admissions criteria” at Pappas, according to nurses there. It is a policy that is likely to lead to Pappas’s closure.
As we have long reported, the administration is similarly allowing the Wrentham and Hogan Centers to die by attrition by denying admissions to all but a handful of applicants in recent years.
The 60-bed Pappas Rehabilitation Hospital in Canton offers medical, rehabilitative, educational and recreational services for persons with developmental disabilities up to the age of 22. In January 2025, Governor Maura Healey did announce that she planned to close the facility in order to save money and move the hospital’s programs to the state-run Western Massachusetts Hospital in Westfield.
COFAR joined state employee unions in opposing the governor’s closure of Pappas. That opposition prodded the administration to reverse its public stance. Healey is now saying she has no plans to close the facility, but the nurses there contend the governor’s statements don’t match the administration’s actual policy.
Last month, staffers at Pappas cast a vote of no confidence in Public Health Commissioner Robbie Goldstein in light of the Public Health Department’s alleged efforts to restrict admissions there, the Boston Herald reported.
Denials of admissions at both Pappas and the ICFs
The administration maintains the allegations of restricted admissions at Pappas are “inaccurate and (an) unhelpful escalation.” But the Herald reported that a mother’s request for admission to Pappas of a 12-year-old boy with severe disabilities had been denied. The boy is nonverbal, blind, and has other medical complications.
The Department of Developmental Services (DDS) has similarly routinely denied requests by family members to gain admission of their loved ones to Wrentham and Hogan. One of those cases involved Kristen Robinson, who is profoundly intellectually disabled, legally blind and quadriplegic, and has a seizure disorder and severe dysphagia, a medical condition that causes an inability to swallow.
DDS initially denied multiple requests by Kristen’s sisters, Kim Meehan and Karen Brady, to get Kristen admitted to the Wrentham Center. It was only through exhaustive efforts that included contacting the media, that Kim and Karen were able to get Kristen into Hogan, where she is now thriving. DDS has continued to deny Kim’s and Karen’s requests to place Kristen at Wrentham, which is much closer to where they live.
It also appears that the legal and internal appeals divisions at DDS have a bias against families and guardians seeking admission of their loved ones to Wrentham and Hogan. In at least two cases, a DDS hearing officer denied appeals by families to transfer intellectually disabled persons from corporate, provider-run group homes to Wrentham.
In both cases, the same DDS hearing officer denied the appeals in rulings that used much of the same language, and discounted concerns raised by the families about a lack of adequate care and meaningful activities in “community-based” group homes and day programs.
In both cases, the hearing officer stated that the individuals did not have a right under federal law to placement in an ICF. Also, in each appeal, DDS stated that it was restricting admissions to ICFs to cases “where there is a health or safety risk to the individual or others, and generally, when all other community-based options have been exhausted.”
COFAR is, as a result, urging state lawmakers to adopt language in the state budget, asserting the right to ICF care for all persons who have been found to be eligible for that level of care.
Rhetoric not matching policy
In the case of Pappas, the administration is insisting that there are no admissions restrictions. The Herald quoted a spokesperson for the governor last month as saying:
Pappas continues to operate as usual, with new patients being admitted and patients being appropriately discharged when they finish their treatment. In fact, the Commissioner has been actively notifying providers of space available for new patients to be admitted at Pappas, and will continue to do so.
At a recent call-in show on Boston Public Radio, Governor Healey made a similarly reassuring statement to a COFAR advocate who asked whether the governor planned to keep the Wrentham and Hogan Centers open. Healey responded, saying, “Rest assured, there are no plans to close any facilities in Massachusetts.”
But the advocate wasn’t given the opportunity on the call-in show to ask any follow-up questions, such as why DDS routinely denies admission to the Wrentham and Hogan centers, and why there has been a steadily declining number of residents, or census, in facilities as a result.
The census at Wrentham dropped from 323 in Fiscal 2012, to 143 in Fiscal 2025 – a 56% drop. The census at Hogan dropped from 155 in Fiscal 2012, to 84 in Fiscal 2025 – a 46% drop.
We are urging all of the advocates for the preservation of Pappas to join us as well in fighting to preserve Wrentham and Hogan. Email or call your House member and urge them to support the upcoming budget amendment establishing a right to care in Wrentham and Hogan. You can find your legislator here.
Saving Pappas and saving Wrentham and Hogan are all a part of the same battle. It is a battle to stop the runaway privatization of state-run care and the race to the bottom in standards that will result from the closure of those state-run facilities.
New book gives a fair-minded account of Walter Fernald, yet unfairly attacks the Fernald Developmental Center
There is a strange dichotomy in a new book by writer and anti-congregate care activist Alex Green about the professional life of Walter E. Fernald, the first superintendent of what was later to become the Fernald Developmental Center.
On the one hand, “A Perfect Turmoil: Walter E. Fernald and the Struggle to Care for America’s Disabled,” offers a largely positive and sympathetic account of Walter Fernald, who took the reins in 1887 of what was then called the Massachusetts School for the Feeble Minded.
Green portrays Fernald as a complex figure—capable of compassion, self-reflection, and change—as he engaged with the flawed scientific ideas of his time.
In contrast, the book paints the Waltham-based Fernald Center itself in a uniformly negative and what we consider to be unfair light, branding it at the outset of the book as “a nightmare” and “a place of shame.” That stark characterization is not supported by a similarly balanced examination of the history of the facility, which functioned until its closure in 2014.
There is no question that institutions like Fernald experienced serious problems, particularly in the early and mid-20th century. But the book gives virtually no attention to the landmark federal litigation in Massachusetts — Ricci v. Okin — which brought about significant improvements, starting in the 1970s, in the care and conditions at Fernald and other developmental centers in the state.
That omission is not a minor one. The Fernald Center remains a potent symbol in the ongoing debate over the future of care for people with intellectual and developmental disabilities (I/DD), including the role of the two remaining congregate care facilities in Massachusetts — the Wrentham Developmental Center and the Hogan Regional Center. By focusing almost exclusively on the Fernald Center’s darkest chapters, the book reinforces a one-sided narrative that continues to shape policy discussions today.
Green has long promoted uniformly negative views about Fernald, the institution. For a number of years, he organized protests and petitions related to the Fernald site, and wrote a commentary in November 2020 that advocated for deinstitutionalization. He was also instrumental in the creation of a state commission in Massachusetts, which made several uniformly negative statements about institutional care in its final report.
Green’s advocacy on these issues is also relevant in light of the book’s selection last month as the winner of the National Book Critics Circle Award in the biography category.
Book lauds Walter Fernald, but disparages the Fernald Center
Here is Green’s description of Walter Fernald, the man, in the introduction to his book:
When (Walter) Fernald died (in 1924)…(h)e was remembered for his compassion and kindness; for having seen a group of people who were otherwise unseen, as individual human beings deserving of our attention, love, and fellowship.
Green also states, later in the book, that:
No figure in American history did more to develop a link between the expert professions that continue to work with the cognitively and developmentally disabled today… Because of his influence on the world around him, (Walter) Fernald’s story is of immense historical significance, but its greatest importance lies in his capacity for self-reflection, self-criticism, and change.
Green does criticize Walter Fernald for his view that intellectual disabilities are inherited, and for being “a master propagandist (and) a moralist prude.” But that criticism pales in comparison to the assessments he makes about Fernald, the institution.
Here is the opening paragraph of the introduction to Green’s book:
The Walter E. Fernald State School is the most important historic site of its kind in the United States. The nation’s foremost institution for intellectually and developmentally disabled people, the school had a life span that stretched across an expanse of time from before the Civil War into the early twenty-first century. But for those who know its name, it does not stir thoughts of dates, places, or events. It is a threat, a nightmare, a deep-seated fear. It is a feeling. A place of shame. Its name is a provocation. It should be.
Here is the first sentence of the second paragraph of the introduction:
Sprawling across 196 acres near Boston, the Fernald School is synonymous with the scandal of human experimentation in the 1950s, of gut-wrenching exposes of abuse and neglect, of the futility of institutionalization and society’s widespread failure to confront that fact.
When it comes to Walter Fernald, Green can clearly be quite complimentary. But when it comes to the facility that Walter Fernald ran, he is relentlessly negative. The question is why. Why not treat Fernald, the institution, with the same open-mindedness and fairness that he treats Walter Fernald?
Fernald, the facility, lasted 90 years after Walter Fernald’s death. It was closed over the objections of the families of its 14 then remaining residents, who filed administrative and court appeals to keep it open. The appeals were ultimately unsuccessful.
Why leave out the positive aspects of Fernald’s history after the 1980s, long after Walter Fernald’s death?
The late U.S. District Court Judge Joseph Tauro noted in his 1993 disengagement order from the Ricci V. Okin case that both the major capital and staffing improvements to the facilities and a program of community placements had “taken people with mental retardation from the snake pit, human warehouse environment of two decades ago, to the point where Massachusetts now has a system of care and habilitation that is probably second to none anywhere in the world.”
Green doesn’t mention that. In fact, he dispenses with Tauro and the Ricci case with one sentence, simply saying that:
In Massachusetts, a series of suits on behalf of inmates, first launched by University of Massachusetts Professor Ben Ricci at the Belchertown State School, were consolidated by Judge Joseph Tauro in federal court, and when Michael Dukakis became governor in 1975, he committed to settling the combined suit by pumping significant sums of money into institutional reform.
Green does not acknowledge Tauro’s conclusion that the reform resulted in a world-class system of both institutional and community-based care. To do so would contradict the narrative that the Fernald Center was never anything other than a nightmare and a place of shame.
Governor asked about Wrentham and Hogan
At a March 27 appearance on Boston Public Radio’s Ask the Governor segment, co-host Jim Braude lauded Green’s book as Governor Maura Healey stood by. Later in the show, Healey took a question from Elaine Strug, a COFAR member and a member of our partner organization, The Saving Wrentham and Hogan Alliance.
Elaine asked whether Healey planned to keep the Wrentham and Hogan Centers open, noting that her son would benefit from the 24/7 specialized medical and clinical care available in either of those facilities. Elaine pointed out that Hogan and Wrentham, which are now known as Intermediate Care Facilities (ICFs), are federally regulated and Medicaid certified.
Healey responded to Elaine, saying, “Rest assured, there are no plans to close any facilities in Massachusetts.” But Elaine was not able to ask a follow-up question as to why individuals like her son are generally denied admission to the centers, and why the administration appears to be letting the centers die by attrition.
Little actual discussion of the Fernald Center
It is also somewhat strange that while Green’s book condemns the Fernald Center, it devotes relatively few of its 368 pages to actually discussing the Center’s sins and shortcomings.
The book instead dwells at length on Walter Fernald’s complex relationship with the eugenics movement in the U.S. and around the world in the early 20th century. Green also extensively discusses Fernald’s shifting views on the nascent intelligence testing movement during that same period. He notes that while Fernald understood the necessity of such testing, he questioned the methodology that was being developed at the time and whether it was accurate in measuring the capacity of persons with I/DD.
Green further discusses Fernald’s skepticism of the push in the early 20th century, in line with the eugenics movement, to sterilize people with I/DD. He quotes Fernald as saying that intellectual disability, which was then called feeble-mindedness “is infinitely a more complicated problem than the believers in the potency of sterilization would have us believe.”
Green’s discussion of those topics is the strongest and most interesting part of his book. There is actually remarkably little discussion in the book of conditions in the Fernald institution itself, even prior to the 1980s.
Green does acknowledge that by the time Fernald closed in 2014, the community-system itself wasn’t living up to the promise that had been envisioned for it. He states that, “group homes became isolating and isolated mini-institutions in and of themselves.”
Green also recognizes that by 2014, the parents of the remaining residents were resisting Fernald’s closure, noting that, “They had fought for improvements to the institution and were getting them. Why should they send people into a world (community system) of cruelty and abuse?”
But then Green dismisses the parents’ concerns:
They were unwittingly in the same position as Walter Fernald in the 1890s, making the argument that had failed him because it deprived disabled people of their fundamental rights as a result of something they were not responsible for – the cruelty of the nondisabled.
Green’s is the standard argument in favor of community-based care: Even if the community system is an isolating system consisting of isolated mini-institutions, disabled people have a right to be subjected to those conditions. Even their families need to understand that this is what is best for them.
And Green flatly states that “the institutions were capable of only so much reform. Rampant abuse was impossible to stamp out,” although he acknowledges abuse is “as likely to occur inside or outside of an institution.” So, why does he condemn only institutional care at the outset of the book?
A book that gets institutional care right
The best history of institutional care I’ve read is Ingrid Grenon’s book, “From One Century to the Next: A history of Wrentham State School and the Institutional Model in Massachusetts.”
As I noted in my review of Grenon’s book, her account of the Wrentham Center makes a powerful case that institutions, in themselves, are neither good nor bad. It is how they are run that counts, just as is the case in any care setting. Grenon recounts that the 1920s was a period when the then Wrentham State School, under the direction of its first superintendent, George Wallace, had a caring staff and administration, and offered a multitude of services and activities for the residents.
As Grenon points out, the Wrentham Center, like Fernald and other similar institutions that sprang up in this state and around the country, entered a long decline, starting in the 1930s as they became more and more overcrowded and understaffed. The state schools in Massachusetts were finally brought back to excellence as a result of the Ricci v. Okin class action litigation.
Unlike Green, Grenon, in our view, draws the correct lesson from history of the role of institutional care in Massachusetts and elsewhere around the country.
Former DDS official asks why an intellectually disabled man can’t get basic services
Ken Moran, a former assistant area director with the Department of Developmental Services (DDS), has been an advocate for Steven Voisine and for Steven’s mother Deborah for several years.
Now living in Florida, Moran still keeps in touch with them, and wants to know why Steven today can’t get the basic services he needs from the Department.
Steven, 37, once had an ideal living arrangement in an apartment with roommates in Lowell. But it all fell apart in 2020, after a DDS-funded corporate services provider allowed a known drug user and dealer to live in the residence.
The drug dealer, whose name was Nick, died of a drug overdose that year. But Ken, and Steven’s mother Deborah, said the provider, the Cooperative for Human Services (CHS), falsely blamed Steven for Nick’s problems; and Steven was forced to move out. Meanwhile, they said, Nick had been stealing Steven’s antipsychotic medications.
No longer getting services
Having lost what had initially been an ideal residential arrangement, Steven went on to live in an array of residential settings, Deborah and Ken said. He experienced temporary homelessness and received minimal case management.
Even though he is 37 years old, he moved into his current apartment in an elderly housing building in Gardner. Ken noted that there is no staff support for him during the day.
Although Steven is under the care of the DDS North Central Area Office in Fitchburg, “They (the area office) don’t know what to do with him or with their other clients,” Deborah maintains. “They just tell us they are overbooked.”
Ken said DDS has most recently offered to find a MassHealth-funded day habilitation program for Steven. But that’s not what he wants or needs.
“He needs someone to actually listen to him,” Ken said. “He needs an apartment with shared responsibilities. He needs someone to help him get his place in order.”
Ken noted that Steven “gets overwhelmed,” is obsessed with electronics, but has no concept of money. He is also unable to keep his apartment clean, and has no social activities or services.
Ken, who is also a former DDS group home licensure and certification inspector, recently retired as chief operating officer of Opportunity Works, a DDS day program provider.
Deborah has track record of accuracy
Ken maintained that Deborah has fought for years for adequate care and services for her son. “Debbie has been pooh-poohed by DDS for years,” he said. “But there is always truth in what she is saying.”
He maintained that Deborah has always tried to alert the Department and providers to potential problems with Steven’s care. One threat she noted was the admission of Nick to Steven’s shared living apartment.
Deborah said Steven had been happiest when living in the Lowell residence with two other DDS clients. Overnight staff stayed on the third floor of the building. There were 20 hours of staffing during the week. But when Nick was admitted, he brought in pot parties, drug addicts, and prostitutes, Deborah said. Ken said Nick had a history of drug abuse and arrests. His mother would bring pot to him.
Steven and Deborah believed Nick was stealing Steven’s medications to sell to drug dealers, so Deborah bought a lockbox for Steven to keep the medications in. They contended DDS knew Nick was a drug user, but still placed him in the apartment.
False accusation against Steven
One day in the fall of 2020, Ken, who had previously retired from DDS, drove Steven to Deborah’s house in Leominster for a weekend visit.
Steven brought his bag of clothes with him in a duffel bag. That Sunday, he called the manager of the shared apartment to ask if he could stay longer, and asked whether the staff could bring his medications to him.
Deborah said that when the manager went into Steven’s room to retrieve his lockbox, she found that the lockbox was gone. The manager called Steven to ask where it was, and he replied that he had left it on his dresser.
Deborah said the staff did a search of the entire building including the garbage and cellar. The lockbox was never found. But the staff nevertheless accused Steven of having taken the lockbox in order to place the blame on Nick for having taken his medications.
Ken and Deborah maintained that accusation against Steven wasn’t true. Steven subsequently had no antipsychotic medications for 10 days, and his psychiatrist wouldn’t prescribe any more.
Nick died of a drug overdose a few months later, in December 2020. Steven’s pill bottles found in Nick’s room when he died, Deborah said.
As noted, Steven was forced to move out of the residence. In our view, this amounted to an eviction by the provider. We think DDS should have informed Deborah of her right to challenge it.
What Steven needs
Ken and Deborah maintain that it wouldn’t be difficult or expensive to serve Steven properly. DDS would need to gain an understanding of his needs. As Ken explained, Steven needs the following services:
- Help managing money
- Help in keeping his apartment clean
- Assistance with hygiene
- Help in making friends
- Help in dealing with depression and weight gain
- Help in dealing with anxiety
- Help with medical and dental care
“He had this kind of support when he lived in Lowell,” Ken said. “He needs good roommates and some staff support. The right living situation could work for him.”
‘The forgotten children’
Deborah said there are many other DDS clients under the care of the North Central Area Office in Fitchburg, who are in the same situation as Steven. “We call them the forgotten children,” she said. She said she was told the service coordinators in the area are overwhelmed. Some have as many as 70 clients.
Both the director of the Area Office and the assistant director have left the office, and have not been replaced, she said. There is currently an acting director.
Deborah said she recently met with DDS Central West Regional Director Anthony Keane, who maintained that the only options for Steven are living by himself or in a group home. Neither option are suitable for Steven, Deborah said.
For the past several years, DDS has become increasingly unable to meet the needs of its clients. Long wait times for services are now the norm.
As we have said before, DDS has been contending with a shortage of staffing and resources, but has not attempted to make use of its existing assets such as the two remaining developmental centers or its state-run group home system. The Department routinely rejects requests for placements in its state-run residential facilities.
When basic services are unavailable for longtime DDS clients like Steven, and when terms like ‘forgotten children’ are used to describe them, it should be a wake-up call to the administration. Unfortunately, this administration appears content to muddle through, and is apparently not listening to many of its clients or aware of what their needs really are.
New report details ‘hidden costs’ in group home care for people with developmental disabilities
Is it really more costly per resident to operate state-run congregate care centers, such as the Wrentham and Hogan centers, than to operate group homes for people with intellectual and developmental disabilities (I/DD)?
That is one of the key assumptions behind decisions by a succession of administrations in this and other states to close state-run Intermediate Care Facilities (ICFs) and move the residents into privatized Home and Community Based Services (HCBS) settings.
But a new cost analysis of ICF versus HCBS group home care in Massachusetts supports previous calls by COFAR to reexamine that assumption. The report, “Hidden in Plain Sight: The True Cost of I/DD Services in Massachusetts and the Case for Restoring Choice,” was produced by COFAR’s partner organization, The Saving Wrentham and Hogan Alliance (The Alliance).
The report makes the overall point that the community-based group home system incurs an estimated $1.3 billion in taxpayer costs each year that are not included in the Department of Developmental Services (DDS) $3.3 billion budget.
COFAR made similar critiques a number of years ago of cost-comparisons issued by the then Patrick administrations to justify decisions to close the former Fernald Developmental Center and three other ICFs.
Today, Wrentham and Hogan are the only two remaining ICFs in Massachusetts, and we are concerned that the Healey administration is letting those facilities die by attrition.
The cost justification for closing the ICFs has been based on comparisons of two line items in the state budget: 1) the community-based residential line item (5920-2000), and 2) the ICF or state facilities line item (5930-1000). But while that analysis provides an accurate account of the cost of serving ICF residents, it is inaccurate as a basis for calculating the cost of serving clients in HCBS group homes.
As the Alliance report explains, ICF costs are bundled into a single rate, which is reflected in the ICF line item in the state budget each year. Those include staffing costs, clinical care, food, housing, and facility costs. All of those costs are included in the state-funded line item for Wrentham and Hogan. The full cost of care is visible in one place.
In contrast, the costs of serving people in group homes show up in several state and federal budgets, including MassHealth, Housing and Urban Development (HUD) subsidies and in SNAP benefits, in addition to the DDS community residential line item. So the argument by ICF opponents that those facilities are more expensive per client than group homes is flawed because only the DDS line item spending per resident is considered in each case.
The Alliance report points out that there are many areas in which spending on group homes occurs outside of the DDS community-based residential line item. A number of those “hidden costs” are calculated in the report, including the following:
- $411 million in day habilitation costs paid by MassHealth
- $385 million–$595 million in medical costs, and $28 million–$75 million in dental costs for adults with I/DD
- $53 million in SNAP benefits
- $33.6 million in transportation costs
- $750,000–$4.5 million in police response to group home crises
The Alliance also discussed a number of other structural reasons for higher-than-expected costs of residential care in HCBS settings, including the high salaries of the executives of corporate residential providers funded by DDS.
A 2022 COFAR survey found that between Fiscal Years 2012 and 2020, total compensation of CEOs, executive directors, and other corporate provider executives in Massachusetts rose from $102.4 million to $125.5 million. That is a 23% increase. Also, the survey found that the average compensation paid per executive rose from approximately $161,000 to $184,000 — a 14% increase.
The Alliance report also found that the HCBS system shifts costs for clinical, medical, and police behavioral responses to cities and towns. HCBS providers are not required to have on-site nursing or medical staff, behavioral crisis responders, or emergency response staff, all of which are provided by ICFs. Instead, the HCBS system relies on calling 911 and on local police, EMS and emergency rooms in hospitals and clinics.
This is why it is misleading to compare the ICF line item with the line item for group homes and divide by the number of residents. A valid comparison must include all major service components, including day habilitation and other supports funded outside the DDS community-based residential line item.
Comparing the DDS ICF budget to multiple budgets that affect group homes leads to the misleading conclusion that the cost of ICF care is higher per resident than group home care, when that isn’t necessarily the case. The Alliance report doesn’t dismiss the ICF costs; rather it says many group home costs are hidden in other budgets, which makes those costs less transparent.
Apples-to-apples cost comparisons are needed
The hidden costs that the Alliance report calculates, some of which COFAR has reported as well, may not prove ICFs are less expensive than HCBS group homes on a per-resident basis, but they effectively rebut the claim that closing ICFs saves money. Without a comprehensive, apples-to-apples analysis, claims of cost savings from closing ICFs are not adequately supported.
The Alliance report makes the reasonable and sensible recommendations to:
- Increase transparency across all funding streams supporting I/DD services, including MassHealth, SSA, HUD, USDA, municipal budgets, and development finance agencies.
- Restore access to state-operated ICF care as a choice for individuals with severe and profound disabilities. COFAR is proposing language in the Fiscal Year 2027 state budget stating that persons found to be eligible for ICF-level care have a right to that care in Massachusetts.
- Reinvest public funds to improve direct care wages, reduce turnover, and strengthen clinical supports.
- Conduct independent audits of HCBS provider finances, real estate holdings, and service delivery practices.
The report correctly concludes that:
Massachusetts’ I/DD service system is far more costly and fragmented than the public budget suggests. By acknowledging hidden costs, restoring balanced service options, and strengthening oversight, the commonwealth can better serve individuals with I/DD, support families, and ensure responsible stewardship of taxpayer dollars.
The Alliance report provides important new data rebutting the argument that state-run, ICF-level care is necessarily more expensive than privatized care.
Key contract documents appear to be missing in DDS guardianship arrangement
Key contract documents appear to be missing involving the procurement of a corporate guardian that has restricted the visitation rights of at least two clients of the Department of Developmental Services.
We have reviewed procurement documents involving TLC Trust, Inc., which has been under a 10-year contract with DDS since 2018 to provide guardianship services to DDS clients. Those documents raise several questions concerning the procurement process.
Neither DDS nor the state comptroller has produced or identified a Master Agreement between DDS and TLC Trust, despite a statement in a DDS guardianship bid solicitation in 2018 that qualified bidders would sign such an agreement.
The bid solicitation, known as a Request for Responses (RFR), also stated that a Procurement Management Team (PMT) would “evaluate proposals in detail and make recommendations for selection.” While DDS did provide the RFR and bid documents submitted in response to it by TLC Trust, DDS did not provide us with any documents reflecting an evaluation of TLC Trust’s bid, beyond a brief award determination.
We previously reported on family visitation restrictions affecting Naomy Alecia and Ryan Moran, two clients for whom TLC Trust has been serving as guardian. We have expressed concerns that those restrictions may be inconsistent with DDS regulations concerning visitation rights.
In December, we asked DDS in a public records request for all current contracts between DDS and TLC Trust. DDS provided only Page 1 of a 5-page Standard Contract Form with the nonprofit organization. That page contained no scope of services or terms and conditions for the provision of guardianship services.
We also asked DDS in January for all bid solicitations and evaluation documents relating to the selection of TLC Trust. As noted, DDS did not produce any evaluation documents.
Because DDS had produced only the first page of a Standard Contract Form, we filed a public records request with the state comptroller in February to find out whether the Comptroller’s Office might have the Master Agreement. On March 5, the Comptroller’s Office responded to our request, stating that it did not have any contractual documents between DDS and TLC Trust to provide guardianship services.
In reviewing the procurement materials that DDS did send us, we also noted the following:
- Of four resumes submitted by TLC Trust in response to the 2018 RFR, only one explicitly referenced guardianship activities, and one did not even reference TLC Trust. At the same time, TLC’s RFR submission stated that the organization had served as guardian to 65 individuals between 2012 and 2018.
- TLC’s RFR response stated that the organization “accompanies individuals for medical care.” In Ryan Moran’s case, his mother reported that TLC Trust has prohibited the family from attending medical appointments.
- The RFR stated that guardians receiving reimbursement under the contract must adhere to DDS’s Standards to Promote Dignity, which include provisions concerning visitation rights. As noted, the cases of Naomy Alecia and Ryan Moran have involved restrictions on family visitation that their families contend are inconsistent with those standards. This raises questions about how DDS monitors compliance with those requirements for guardians operating under the contract.
No answers to questions
On March 4, I emailed DDS Commissioner Sarah Peterson, asking the following questions:
1. Did DDS execute a Master Agreement with TLC Trust pursuant to the RFR? If so, where is that agreement kept?
2. Were detailed evaluation materials created of TLC Trust’s RFR submission? If so, can DDS confirm their existence?
3. Did DDS verify TLC Trust’s representation that it was serving as guardian to 65 individuals as of 2018?
4. Which TLC Trust employees have served as guardians of DDS clients since 2018, and what is the approximate client caseload per staff member?
5. How does DDS assess whether guardians receiving reimbursement under this contract are adhering to the Standards to Promote Dignity referenced in the RFR?
To date, I have not received a response from Peterson or the Department to my questions.
Lack of information raises further questions
A lack of answers and information from both DDS and TLC Trust only raises further questions and confusion about the organization’s role and qualifications.
In January, I emailed Gayle Greene, executive director of TLC Trust, and Diane Parker, who is listed as a case manager there. I noted that we were urging TLC Trust to ensure that their visitation policy conforms to the Department’s regulations, and we were asking that they re-examine and remove any visitation restrictions that have been placed on these two families. We believe these restrictions are causing stress and hardship to Naomy and Ryan and to their families.
I also asked how many DDS clients TLC Trust currently provides guardianship services for. We have reported that payments from DDS to TLC Trust from Fiscal Year 2022 through the current fiscal year have totaled $532,000. That averages out to close to $125,000 a year for the four full fiscal years from 2022 to 2025.
Both Greene and Parker are listed in court documents as performing guardianship services to Ryan Moran. Naomy’s mother, Lizvette Rivera, said Parker was providing guardianship services to Naomy. Neither Greene nor Parker responded to my January email query.
Despite the lack of mention of guardianship experience in most of the resumes submitted to DDS, TLC Trust stated in a one-page description of the organization’s history and qualifications that it started providing guardianship services to DDS clients in 2012, and was providing those services as of 2018 to 65 people. The one-page description added that:
Staffed by an Executive Director and three case managers (resumes attached), we consider ourselves “hands on” guardians. …DDS refers to TLC Trust on average between two and five new individuals per month for guardianship services. We have come to be known as an agency that will provide services to individuals who have dual diagnosis and whose situations could be described as “difficult”.
Given that only one of four resumes mentioned guardianship experience as of 2018, TLC Trust’s claim that it was providing those services to 65 people as of that year raises questions about the quality of those services and who was actually providing them.
We have urged DDS to investigate TLC Trust’s actions as guardian to Naomy and Ryan.
The RFR stated that DDS would reserve the right to remove any selected guardian if the guardian’s “conduct should fall below that expected of a fiduciary at the Department’s and the Court’s discretion.” In our view, in restricting family visitation, TLC Trust has displayed conduct that appears to fall below that expected of a fiduciary.
However, given that there is no complete contract that has been produced in this case, we don’t know whether such a contract contains a term similar to the RFR in which DDS reserves the same right to remove TLC Trust.
In an editorial today, The Boston Globe decried the state’s poor track record in responding promptly to public records requests, and in providing information to the public in general. As the Globe noted, “Well-managed public entities should certainly be able to respond to requests for information in a reasonable amount of time, at a reasonable, or no, cost.”
Unfortunately, there seems to be no better example, in our experience, of this disinterest in transparency in government than the Massachusetts Department of Developmental Services.