DDS and group home deny responsibility for month-long family hospital visitation ban
The Department of Developmental Services (DDS) and a department-funded group home provider are denying responsibility for having blocked a group home resident’s family from visiting him at Brigham and Women’s Hospital for more than a month, starting in January.
The hospital is not commenting on the matter and has been unresponsive to numerous attempts by COFAR to inquire on behalf of the family about the justification for the blocked visitation. The hospital has even declined to clarify its general visitation policies.
Meanwhile, the resident’s DDS-funded guardian and the Seven Hills Foundation, the group home provider, appear to be continuing to impose restrictions on family visits to the group home. Those restrictions appear to violate DDS regulations.
As we previously reported, the family of Giovanny Arias, an individual with autism spectrum disorder and other conditions, was prevented from visiting him in the hospital where he was taken after having reportedly fallen down the stairs of his group home on December 19. He suffered injuries, including a broken wrist, black eye, and numerous bruises throughout his body.

Giovanny Arias and his grandmother, Liduvina Gonzalez
Due to the visitation restrictions, the family was deprived of information about Giovanny’s well-being and whereabouts for over a month while he underwent numerous surgical operations, his great aunt, Carolina Hernandez Broomhead, said.
The ban on visiting Giovanny in the hospital followed growing communication and visitation restrictions imposed by Seven Hills management and Giovanny’s state-paid guardian, Susan Braus, in the group home, Carolina said. Carolina contended the restrictions started after the family expressed concerns about insufficient care at the group home.
Visitation restrictions appear to be a part of a pattern in which families are marginalized when they attempt to advocate for their loved ones (see here, here, here).
Previous visitation restrictions at the residence
Issues involving visitation restrictions in Giovanny’s group home first arose this past fall. Carolina contended that Seven Hills and the guardian had responded with visitation restrictions against the family for having alleged that the group home was subjecting Giovanny to poor hygiene and overmedication, and had depleted his Social Security funds. Seven Hills also prevented Giovanny’s grandmother from seeing her grandson at the residence, and, at one point, even called the police on the seventy-eight-year-old woman, Carolina said.
Moreover, in November, Seven Hills proposed a series of new restrictions that included a ban on family visits to the residence. Family visits would have to occur at other predetermined locations. There would also be a maximum of two family visits per month with a limit of two hours per visit. Additionally, the family would be required to bring a translator with them on all visits for the benefit of staff who are unable to speak Spanish. A fuller discussion of the restrictions is available here.
Withheld medical updates on the evening of the hospitalization
Existing tension surrounding mistreatment and visitation limitations appeared to escalate during Giovanny’s hospitalization, starting on December 19, at Brigham and Women’s Hospital.
That night, Carolina said, she participated in a three-way phone call with a doctor and Braus. She said she heard Braus direct hospital personnel to withhold medical information from the family, even as a doctor recommended otherwise. Consequently, the family was denied vital information about Giovanny’s welfare amid a health emergency, she said.
Family hospital visitation restrictions
Hospital visitation restrictions soon ensued after Giovanny’s admission. While the family was permitted to visit Giovanny at the hospital on December 31, visitation was suddenly restricted on January 2, Carolina said. That day, two security officers unexpectedly ushered another aunt out of the hospital after she attempted to visit Giovanny. Carolina said they did not provide any explanation for the aunt’s removal.
Family difficulties accessing information about hospital visitation restrictions
Shortly afterwards, Carolina called the hospital for more information on the incident. She said a Brigham and Women’s employee claimed to her that Braus had submitted written documentation barring family visits. Carolina said that when she followed up with Braus, however, Braus claimed the hospital was responsible for the visitation ban.
Other attempts by the family to receive clarification of the visitation restrictions in the hospital have been futile, according to Carolina. In an email dated January 13, DDS area director Jeffrey Hetrick claimed that neither DDS nor the guardian had a say in the restrictions, and placed responsibility on the hospital.
Seven Hills Area Director Caelin Scribner similarly asserted that Seven Hills was uninvolved in the decision-making process on visitation, and maintained the hospital alone made the decision to deny family visits. In their emails, both DDS and Scribner encouraged the family to contact the hospital for clarification. Yet, further family outreach to the hospital was unsuccessful, Carolina said, with the hospital hanging up the phone and not responding to emails.
COFAR difficulties assessing responsibility for hospital visitation restrictions
COFAR also experienced similar challenges while investigating the situation. Neither Braus nor Scribner replied to our emails requesting clarification on the hospital visitation restrictions. We emailed DDS Commissioner Sarah Peterson on January 8 to express concerns about the family hospital ban and were told that the DDS Area Office staff would follow up with the family directly. We reached out again on January 26 to the commissioner to highlight that the issue remained and have yet to receive a response.
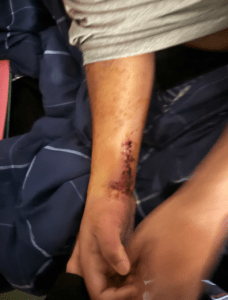
Giovanny’s broken wrist, which the provider claims he suffered after falling in the group home in December.
Communication with the hospital has proven difficult as well. Despite having a seven-day response timeframe, the hospital didn’t respond to three of our emails about the restrictions. The Brigham and Women’s Patient and Family Relations Department finally replied to us in a January 26 email, stating we would need “a release of information signed by someone who has the authority to speak for the patient.”
While laws protecting health information may limit the public’s ability to receive case details, even our request for basic clarification on hospital visitation policies was not answered by the hospital.
On January 26, I called the floor where Giovanny was hospitalized and was told by a hospital staff member that they could not give me any information and that I would need to speak with Braus instead.
When I clarified that I simply had general questions about the hospital visitation policy, the staff member offered to connect me with a supervisor. After leaving me on hold for about twenty minutes, the staff member returned and said I would have to contact the Patient and Family Relations Department. When I asked if I could speak to the supervisor, the staff member responded that they did not have that person’s contact information.
Implications of the family hospital visitation restrictions
Regardless of who initiated the hospital restrictions, it is concerning that all parties have disclaimed responsibility rather than working to resolve the problem. Each entity has a duty to promote Giovanny’s best interest in partnership with the others.
Isolating an individual with disabilities from his family for over a month cannot be said to advance his best interest. For a person with autism who has limited abilities to communicate with speech, the disruption of routine and exposure to an overwhelming sensory environment in isolation could be traumatic.
The hospital family visitation restrictions seem to be inconsistent with Brigham and Women’s own Patient Rights statement. This affirms that patients have the right to “communicate with people outside of the hospital” and “participate in [their] care.”
The family visitation restrictions also appear to violate Giovanny’s legal rights. His 2024 legal guardianship decree states that Giovanny retains the right “to determine with whom to have friendships and visitation.” No one has claimed that the restrictions stem from Giovanny’s preferences, Carolina said.
Recent hospital discharge and continuing visitation limitations at the group home
In a February 6 email, Braus stated she believes that Giovanny would actually enjoy family visits.
When Giovanny was finally discharged from the hospital recently, Scribner and Braus separately reached out to the family to discuss arranging a visit at the group home. In Braus’ email she commented that she would “imagine [that Giovanny] would appreciate a family visit during his continued recuperation.” According to Carolina, this raises the question why Braus did not intervene to address the month-long hospital visitation restrictions.
Scribner, meanwhile, offered to host a two-hour-long family visit that Sunday with a maximum of two visitors so that Giovanny could “enjoy time with loved ones while still prioritizing his recovery.” She said that future group home visits could not exceed two visitors and would need to have attendees approved by Braus ahead of time. Carolina said it appears that the group home has imposed its November 2025 proposed visitation restriction agreement despite the fact that it was never signed by the family.
In our view, Braus and Seven Hills’ sudden allowance of a group home visit does not negate possible DDS regulation violations. The regulations state that “arrangements shall be made for private visitation to the maximum extent possible” and “family members shall be permitted to visit at all times, unless the individual objects.” Permitting visits sporadically and subjecting visitation to onerous terms and conditions amid growing backlash cannot be said to adhere to the spirit of the regulations.
The hospital visitation restrictions demonstrate the ease with which families can be dismissed and ultimately excluded by major players in the DDS-funded, provider-run residential system. When responsibility is diffused across state agencies, state-paid guardians, and corporate providers, accountability dissolves. Families are reduced from key team members to outsiders while their loved ones with disabilities suffer the fallout.
DDS line items would get small increases while some MassHealth accounts would see cuts under governor’s FY ’27 budget
Governor Maura Healey has proposed relatively small increases in the Department of Developmental Services (DDS) budget for provider-run group homes, state-operated group homes, and for the Wrentham and Hogan Centers in the coming fiscal year, which starts July 1.
However, some of the state’s largest MassHealth accounts would face cuts under the governor’s budget proposal, raising the possibility of cuts in funding for Day Habilitation and Adult Foster Care programs and Personal Care Attendants for persons with intellectual and developmental disabilities (I/DD).
MassHealth is Massachusetts’ Medicaid program, through which the state administers and receives federal Medicaid reimbursement.
There appears to be no indication yet that the state’s 50% Medicaid reimbursement level from the federal government will be cut. But there have been proposals at the federal level to do so. At the same time, the Trump administration and Republicans in Congress have maintained the cuts won’t affect people with I/DD.
On January 28, Healey unveiled a $62.8 billion proposed budget for Massachusetts for the coming fiscal year. The governor’s budget legislation has been sent to the state Legislature’s House Ways and Means Committee; and from there it will proceed to votes in the full House and Senate.
Among the DDS line items we are concerned about are the following:
- The Wrentham and Hogan Intermediate Care Facilities (ICFs) (Line item 5930-1000):
Healey has proposed a $4.6 million, or 3.5%, increase in this line item, bringing it from $129.7 million to $134.3 million.
Despite that increase, we remain concerned that the Wrentham and Hogan Centers are being allowed to die by attrition, given that the administration routinely denies admission to them. Since Fiscal Year 2012, the ICF line item has been cut by more than $18 million, or more than 12%.
We visited the House Ways and Means and other key committees at the State House yesterday, asking them to support proposed language in the ICF line item that we think would open those facilities to new admissions. Our proposed language states that persons eligible for ICF-level care in Massachusetts have a right to that care.
- State-operated group homes (Line Item 5920-2010):
The governor has proposed a $25 million, or 7.2%, increase in this line item, which funds state-operated group homes. The increase would bring projected spending of $347.2 million in the current fiscal year to $372.3 million next year.
We believe the administration, while proposing modest increases in this line item, is also effectively allowing the state-run group home network to die by attrition. The data coming from DDS is inconsistent, however, regarding the trend in the total number of residents, or census, in those facilities.
The latest census data provided by DDS in September has produced confusion over whether the total census in state-operated group homes has been rising or falling. Data provided by DDS in previous years consistently showed the total census had been steadily falling. However, the new data set from DDS in September indicates that the census actually rose during the same fiscal years DDS had previously said it was falling – 2020 through 2023.
It seems most likely to us that the census in the state-operated homes has been steadily falling. We have heard that several homes have been closed in recent years, that staffing has been cut, and that it is difficult, if not impossible, to gain admission to those residences.
- Corporate provider-run group homes (Line Item 5920-2000)
The much larger corporate-provider-run group home system would receive a 2.4%, or $48.5 million, increase under the governor’s budget proposal, to $2.07 billion. While that increase is relatively modest, the provider line item has been on an entirely different funding trajectory for the past two decades than has the ICF line item. Since Fiscal 2012, the provider line item will have been increased by $1.3 billion, or 173 percent.
MassHealth programs would be cut
The Arc of Massachusetts, a key lobbying group for the corporate providers, is reporting that the MassHealth budget would see an across-the-board rate freeze, under Healey’s budget. According to the Arc, the proposed budget also includes significant cuts to Adult Foster Care, Personal Care Attendants, and Adult Day Health programs.
However, given that these programs are funded through large accounts, it’s not clear how much those specific services would be cut if the governor’s budget is adopted.
Healey has proposed cuts in the following MassHealth accounts:
- MassHealth Medicaid Administration (Line Item 4000-0300):
This account, which includes funding for Personal Care Attendants, would be cut by $3.2 million, or 2%, from $159.4 million to $156.2 million.
- MassHealth fee-for-Service (Line Item 4000-0700):
This account, which funds Adult Foster Care and Day Habilitation programs, would be cut by $268 million, or 6%, from $4.4 billion to $4.2 billion.
- MassHealth managed Care (Line Item 4000-0500):
This account, which also funds Adult Foster Care and Day Habilitation programs, would be cut by nearly $1 billion, or 14.2%, from $7 billion to $6 billion.
Many questions loom over the planned cuts in federal funding, particularly over the impact those cuts will have on people with intellectual and other disabilities. But over the long term, perhaps a more fundamental question is what will the Healey administration’s policy of promoting privatization of services mean for the future of Wrentham, Hogan, and other critically important state-run facilities and services for some of our most vulnerable citizens.
Even if Massachusetts is spared from devastating cuts in Medicaid reimbursement, the ongoing trend toward the closures of the ICFs and state-run group homes will still result in a race to the bottom of care for those persons in this state.
DDS has minimal contractual documentation regarding corporate guardian that has supported severe visitation restrictions on two families
The Department of Developmental Services (DDS) has produced only one page of an apparently larger contract with a corporate guardian that has supported severe visitation restrictions on two separate families.
TLC Trust, Inc., which was hired by DDS in 2018 as a guardian of at least two group home residents, has continued to support restrictions on family visits to them. We have raised concerns that the restrictions violate DDS regulations that establish visitation as a right of both DDS clients and their families.
Payments from DDS to TLC Trust for the past five years for providing guardianship services have totaled $532,000, according to information provided by DDS under a Public Records Law request. That averages out to close to $125,000 a year from Fiscal Years 2022 to 2025. (Several years ago, we investigated DDS’s secretive system for paying professional guardians.)
In response to our Public Records request for all contract documents with TLC Trust, DDS last month provided only what appears to be Page 1 of a 5-page “Standard Contract Form” with the organization for guardianship services.
While the contract page refers to a “brief description of contract performance” and a “detailed description of contract scope…,” neither a contract performance description nor a contract scope description was provided in DDS’s response. The contract page also refers to a “Master Agreement Contract with standard rates.” That was not provided either.
On January 14, we appealed to the state’s Public Records Division, arguing that the DDS response appeared to be incomplete. On January 28, DDS responded to our appeal, stating that the Department has no further responsive records. That same day, the state Public Records Supervisor closed our appeal.
There are questions about the competitive solicitation process used in selecting TLC Trust to provide guardianship services. We have filed a new Public Records request with DDS for all procurement documents involving TLC Trust, including Requests for Proposals (RFPs) and evaluations of responses.
It appears DDS issued a Request for Responses (RFR) for guardianship services in 2018 or 2019, and TLC Trust appears to have been among the respondents. However, DDS has not provided TLC Trust’s response, qualifications materials, or any evaluation or award documentation.
Severe visitation restrictions continue
We previously reported that TLC Trust, Inc., appeared to have been involved in preventing the families of Ryan Moran and Naomy Alicea from visiting them on Thanksgiving Day last year. The families were similarly prevented from visiting Naomy and Ryan at Christmas.
The families maintain in each case that the visitation restrictions resulted from their complaints that their loved ones have been subjected to abuse or neglect in their provider-operated residences.
Naomy, 37, has an intellectual disability (ID) and cerebral palsy. Ryan, 29, has ID and is on the autism spectrum. DDS placed Ryan in a group home run by Venture Community Services in 2020, when he was 24. Naomy has been living in a separate group home in Worcester, which is operated by the Seven Hills Foundation. Both Venture and Seven Hills are DDS-funded residential providers.
Members of both families contend that their guardianships of their loved ones were removed for questionable reasons. DDS successfully petitioned the Worcester Probate Court to appoint TLC Trust as the corporate guardian of Ryan and Naomy.
Since 2022, Gayle Greene, Executive Director of TLC Trust, and Diane Parker, identified on TLC Trust’s website as a case manager, have provided guardianship services to those individuals on behalf of TLC Trust, according to Worcester Probate Court records.
Naomy’s mother, Lizvette Rivera, said last month that she was allowed to see Naomy only twice that month. She was not allowed to visit her at her group home.
Ryan’s mother, Hilda Natal, said she and Ryan’s father, Jose Moran, have been barred from visiting him since early October for reasons that were never specified. While that ban was supposedly ended on January 9, it is still not clear when visits will be allowed to resume. They said DDS and Venture officials told them they would be allowed one supervised visit a month, but, “We were told it could be February or March,” Hilda said.
We believe the visitation restrictions violate DDS regulations, which state that DDS clients have the “right to be visited and to visit others under circumstances that are conducive to friendships and relationships.” Also, the individual’s family members “shall be permitted to visit at all times, unless the individual objects…”
Commissioner and TLC Trust contacted
In November, I wrote to DDS Commissioner Sarah Peterson to urge that DDS allow Ryan’s family to visit him on Thanksgiving Day. Since then, we learned that a similar prohibition on visits had been imposed on Naomy’s parents, and that TLC and Parker were involved in each case in imposing the restrictions.
In December, Peterson responded, saying she had “followed up with the local teams on the specifics of these cases. While I know you understand that I cannot comment on specific cases, please be assured that they are engaged and will follow up,” she wrote.
Both Hilda and Lizvette said no one from DDS has contacted them since December to discuss their concerns.
On January 27, I emailed Greene, executive director of TLC Trust, and Parker. I urged them to ensure that TLC’s visitation policy conforms to the Department’s regulations, and that they re-examine and remove the visitation restrictions on the two families.
I also asked Greene and Parker whether TLC had responded to a competitive solicitation from DDS to provide guardianship services in these and any other cases. To date, I haven’t received a response from them.
TLC contract issues
The single contract page for guardianship services from TLC Trust that DDS provided to us was signed by Greene in February 2018. Peterson was listed on the contract page as the contract manager. Peterson became commissioner of DDS last April. In 2018, she was serving as a deputy general counsel for DDS.
In her response to us in December, Peterson maintained that “TLC Trust qualified through state procurement procedures to receive and accept appointments from DDS.”
But given the lack of DDS’s contract documents, there appear to be questions about the bid solicitation process.
In DDS’s original response to my Public Records request, the Department provided a link to its RFR information on the state’s online COMMBUYS site. COMMBUYS is the state’s electronic posting and bidding system for goods and services. It is operated by the Operational Services Division (OSD).
The RFR did describe the scope of what it said is a master agreement that winning bidders must sign, and stated that bidders must state their qualifications. However, as noted, DDS did not provide us with TLC’s response to the RFR. The RFR requested respondents to list their qualifications to provide guardianship services, among other information.
As a result, we filed new Public Records requests last week with both DDS and OSD for all procurement documents that relate to the selection of TLC Trust for guardianship or professional guardian services.
On January 29, I received a response from OSD that they did not have any procurement documents involving TLC Trust. That leaves DDS, which has until February 9 to respond to us, under the Public Records Law.
We also filed a separate Public Records request last week with the state comptroller for possible contract records concerning TLC. The one contract page that DDS provided states that, “Commonwealth Terms and Conditions (T&C) has been executed filed with CTR (the state comptroller) and is incorporated by reference into this Contract.”
As we’ve said previously, it is unclear why TLC was appointed as guardian of these clients. TLC’s website states that the organization primarily administers trusts with a minimum value of $100,000 for persons with developmental and other disabilities.
While the TLC website says the organization can also act as a corporate guardian for persons, the website further states that, “First priority for this (guardianship) service will be given to those individuals who have a trust relationship with the organization.” No such trust account with TLC exists in either Ryan’s or Naomy’s case.
Given that there was a competitive procurement process used in hiring TLC Trust to provide guardianship services, it will be helpful to know what TLC Trust’s qualifications are, what its response was, and how DDS evaluated it. If there are no such documents that can be produced, that would raise even more questions about this matter.
DDS withholds information on investigation of its data on the census of state-operated group homes
In the wake of questions raised by COFAR, the Department of Developmental Services (DDS) appears to have conducted an internal investigation of its apparently contradictory data on the total number of residents in its state-operated group homes.
The Department, however, has declined to provide any records of that investigation to us, citing attorney-client privilege. An attorney for the Department, meanwhile, has not responded to a query I sent her on the matter on January 5.
As we reported last fall, a new set of census data provided by DDS in September has produced confusion over whether the total number of residents, or census, in state-operated group homes has been rising or falling. Data provided by DDS in previous years consistently showed the total census of the homes had been steadily falling.
However, the new data set from DDS in September indicates that the census of the state-operated homes actually rose during the same fiscal years DDS had previously said it was falling – 2020 through 2023. Moreover, the new data show the census continued to rise until as recently as last year. (See graph below depicting the two contradictory sets of data from DDS.)
The DDS state-operated group home network is far smaller than the privatized group home system, which is managed by DDS-funded corporate providers. However, we consider the state-operated homes to be critically important in maintaining the fabric of care in the DDS system.
DDS spends about $350 million a year in operating its state-run group homes, compared with more than $2 billion a year on the provider-operated homes. We are concerned that the Healey administration is allowing the state-operated group home network to die by attrition.
Due to the apparent discrepancy in the data, we filed a Public Records Law request with DDS on November 13 for documents pertaining to apparent changes made by the Department to its census data for state-operated group homes between Fiscal Years 2020 and 2023.
DDS responded to us on December 29, indicating that they had located 74 internal emails and email attachments that were responsive to our records request. But an assistant DDS general counsel stated that, “All responsive records, including emails and email attachments, are withheld on the basis of the attorney-client privilege.” Each email involved a communication between a DDS attorney and another DDS official or attorney.
Subject matter listed as ‘investigation’
A document provided by the assistant general counsel as part of the December 29 response provides brief descriptions of the subject matter of each of the emails that were considered responsive. For 36 of the 74 emails and attachments, the subject matter is described as “Communication re: investigation of PRR census data for counsel.” (my emphasis)
The document provides no explanation as to what is meant by “investigation” or what aspects of the census data were or are being investigated.
On January 5, I emailed the assistant general counsel, asking whether DDS has opened an investigation of the apparent changes made in its census data for state-operated group homes, specifically for Fiscal Years 2020 through 2023. I also requested an explanation for the contradictory nature of the two sets of data. To date, I haven’t received a response to my query.
Appeal denied
As the graph above shows, DDS provided contradictory sets of data in two responses to our public records requests in November 2023 and September of last year. The largest discrepancy in the data concerns Fiscal Year 2020, for which the 2023 DDS response listed the total census of the state-operated homes as 1,026, while the 2025 response listed the total census as 857.
The graph further illustrates how that difference of 169 residents in the two data sets for Fiscal Year 2020 established two contradictory trends in the data from that year onward. The solid red line representing the 2023 DDS response shows a downward trend in the census, whereas the dashed green line representing the 2025 response shows an upward trend.
As as result of that discrepancy in DDS’s responses, we filed an appeal with the state Public Records Division last September, asking asking the public records supervisor to direct DDS to clarify or reconcile its two sets of census data, or to explain in writing the reasons for the discrepancies so that the records provided would be comprehensible and complete.
On October 6, the Public Records supervisor denied our appeal, contending we hadn’t alleged a “clear violation” of the state’s Public Records Law by DDS.
On October 14, we asked the Public Records supervisor to reconsider her denial. We noted that by producing two conflicting sets of census data for overlapping fiscal years, DDS had failed to demonstrate that it had furnished the actual records it maintains as required by the Public Records Law.
On October 31, the Public Records Supervisor denied our request for reconsideration without responding to our argument about the failure to assist in meaningfully identifying the records we had received. She stated only that, “There is a presumption that public officials perform their duties in an honest and impartial manner.”
As a result of the denials of our appeal and request for reconsideration, we filed the November 13 public records request, asking for all documents pertaining to the apparent changes in the census data.
Administration’s secrecy reduces public trust
So far, the only thing we have learned from this whole exercise is that DDS may have conducted, or may be conducting, an investigation of some kind regarding that data. As usual, the Department appears to have found a way to prevent the public from learning what is actually going on.
This is particularly unfortunate given that the Department’s secrecy prevents the public from knowing a basic fact about the future of the state-operated group home system and by extension state-run services in general. Whether the census in the group home system is rising or falling has direct implications for the system’s viability in coming years.
Despite the September data that was provided to us, it seems most likely to us that the census in the state-operated homes has been steadily falling. We have heard that several homes have been closed in recent years, that staffing has been cut, and that it is difficult, if not impossible, to gain admission to those residences.
In July 2024, we reported that Governor Maura Healey had cut more than $400,000 from her proposed funding for state-operated group homes in the Fiscal Year 2025 budget. That cut resulted in final funding for the homes that was $2.4 million less than the governor’s initial proposal, despite an overall 4% increase from the previous year.
A year later, we reported that the Legislature had adopted a lower funding increase for the state-operated homes for Fiscal 2026 than what the governor originally proposed. The Legislature instead prioritized the larger corporate-run system, as usual.
These occurrences are not a prescription for a rising census in the state-run group homes. Yet DDS’s latest data say that is just what happened, without offering an explanation for it.
We continue to fail to understand why the administration feels it is necessary to withhold vital information like this from the public. We don’t see how anyone benefits from a policy that reduces the public’s trust in government.
Family, blocked from visiting group home resident, also barred from visiting him in hospital
A resident of a group home suffered serious injuries there requiring hospitalization, and now his family is barred for undisclosed reasons from visiting him in the hospital.
Late last month, Giovanny Arias, who has autism spectrum disorder and other conditions, reportedly fell down a flight of stairs in the group home, according to his great aunt, Carolina Hernandez Broomhead. The Roslindale home is run by the Seven Hills Foundation, a corporate residential provider funded by the Department of Developmental Services (DDS).
Giovanny’s injuries included a broken wrist, black eye, and numerous bruises across his body, according to Carolina.
While Giovanny has undergone two surgical operations at Brigham & Women’s Hospital in Boston, his family has been prohibited from visiting him there and has been denied medical updates, Carolina said.
The ban on visiting the hospital follows mounting communication and visitation restrictions imposed by the Seven Hills management and by Giovanny’s state-paid guardian, Susan Braus, Carolina said. She said the restrictions began after the family complained of inadequate conditions and poor care at the residence.
Seven Hills even prevented Giovanny’s grandmother from seeing her grandson and, at one point, called police on her, Carolina said. She said Giovanny has been subjected at the residence to poor hygiene and overmedication, and to the disappearance of his Social Security funds.
Seven Hills has not provided the family with an accounting of his monthly spending, and has claimed he has no money. Carolina said her family has had to supply all of Giovanny’s clothes, blankets, mattresses, and bed linens, and has had to provide food for him on a weekly basis.
Carolina also said that in November, Seven Hills proposed a series of additional restrictions, including a complete ban on family visits to the group home. Family visits would have to take place at other agreed-upon locations. There would also be a cap of two family visits per month with a maximum duration of two hours per visit.
In addition, the family would be required to bring a translator with them on all visits for the benefit of staff who are unable to speak Spanish. We believe this requirement violates DDS regulations that establish a right of clients to have confidential communications and demonstrates a lack of sensitivity to culturally diverse communities.
As we have been reporting, staff neglect and restrictions on family visitation often go hand in hand in DDS-funded group homes (see here).
Restrictions on visits
According to Carolina, Seven Hills management, DDS, and Braus have blamed the family for failing to act in Giovanny’s best interests. Before his hospitalization, over 100 days had passed since Giovanny last saw any member of his family apart from a single cousin, Carolina said.
Carolina said the Seven Hills group home management blocked Giovanny’s grandmother, Liduvina Gonzalez, from visits and communication with Giovanny after she complained about substandard food and inadequate hygiene. The Seven Hills management called the police on the 78-year-old woman after she attempted to visit her grandson on September 21.
The restrictions appear to violate a 2024 decree naming Braus as Giovanny’s guardian. The decree states that Giovanny retains the right “to determine with whom to have friendships and visitation, with assistance if needed.”
Family response
In response to the alleged neglect and visitation restrictions, Carolina delivered what she termed a “demand letter” on behalf of the family to DDS on November 5. In the letter, she called for inspection and remedy of Giovanny’s current care conditions, his relocation to a more suitable setting, and restored family visitation and communication rights. The rights included regular, in-person visitation and private telephone or video calls at reasonable and scheduled times.
The family has yet to receive any reply to the letter, Carolina said. She said Giovanny’s DDS service coordinator, James Griffin, has ceased responding to her communications since she sent the letter.
Rather than opening a dialogue with DDS and Seven Hills about how to better support Giovanny, the demand letter sparked a wave of new visitation restrictions, according to Carolina. She also said Griffin has excluded her from all meetings related to Giovanny.
Seven Hills visitation restriction agreement
On November 14, the family received a proposed agreement that DDS, Seven Hills, and Braus requested that they sign, listing rigid requirements for family visits and communication with Giovanny. The restrictions include the following:
In-person visits:
- Family visits cannot occur at the group home and can only be scheduled for outside locations agreed upon by both parties in advance.
- Family visits may occur only twice per month on Sundays and must be planned at least a week in advance.
- Family visits are limited to a maximum duration of two hours.
- If a family member needs assistance with personal care, they cannot visit unless accompanied by someone who can provide assistance.
- The family must have an individual present at all visits to translate for the benefit of the staff if the visiting family member is unable to communicate in English. There cannot be more than two people present during any visit.
- Family members are not permitted to bring food to Giovanny under any circumstances.
- Seven Hills can terminate visits at any point they deem “appropriate.”
Phone calls:
- The family can call Giovanny only on Tuesdays and Thursdays after 3 p.m. If Giovanny declines the phone call, the family is not to call back.
- The family is not permitted to call staff or discuss problems unless they are able to speak English or have a translator on the line.
- If at any point in time, the family’s behavior is deemed “negative,” Seven Hills has the right to hang up on the call with notice and organize another time to call with DDS involvement.
Questionable provisions of the restriction agreement
Several of the provisions of the proposed agreement appear to be in violation of DDS regulations, which state that DDS clients have “the right to be visited and to visit others under circumstances that are conducive to friendships and relationships,” and that “family members shall be permitted to visit at all times, unless the individual objects.”
The regulations note that “reasonable restrictions” may be placed on the time and place of visits “to protect the welfare of the individual or the privacy of other individuals and to avoid serious disruptions in the normal functioning of the provider.” However, the regulations require that arrangements be made “for private visitation to the maximum extent possible.”
There is no indication that Giovanny’s family visits have ever adversely affected Giovanny or other residents to warrant such restrictions. The restrictions limiting the number, duration, eligible participants, and locations of visits can hardly be considered to allow for private visitation “to the maximum extent possible.”
We are further concerned by the restrictions’ failure to accommodate the needs of linguistically diverse families. The requirement that family visits occur exclusively in English not only limits meaningful expression that preserves a sense of cultural identity, but also impedes private conversations amongst family members. This also appears to violate DDS regulations, which state that DDS clients maintain “the right to communicate,” including “the opportunity to make and receive confidential communications.”
Escalating health concerns
Carolina said issues involving neglect and visitation restrictions reached a breaking point on December 19, when Giovanny was hospitalized at Brigham and Women’s Hospital.
During a three-way telephone call with a doctor and Braus on the evening Giovanny was hospitalized, Carolina said, she heard Braus instruct hospital staff to withhold medical updates from the family, even as a doctor suggested that the information be shared. As a result, the family was deprived of critical information about Giovanny’s health during a medical emergency, she said.
Family visitation restrictions amid medical crisis
Although the family was able to visit Giovanny in the hospital on December 31, they were barred after that from visiting him there, according to Carolina. On January 2, two security officers escorted another aunt out of the hospital after she attempted to see Giovanny, Carolina said.
When Carolina called to inquire about that incident, a Brigham and Women’s staff member told her Braus had submitted written documentation restricting family visitation, Carolina said. She said that when she spoke with Braus, however, Braus denied this and attributed the restrictions to the hospital.
DDS response
We emailed DDS Commissioner Sarah Peterson on December 1, asking the Department to investigate the allegations of neglect at Giovanny’s group home and to allow unrestricted family visits. We were later told that a DDS official would be reaching out to the family directly to address these issues. But Carolina said as of January 6 that no one had contacted her.
The coexistence of neglect and visitation restrictions has been an undercurrent in many of the cases brought to our attention (see here, here, and here), particularly when DDS involves itself in guardianships or co-guardianships.
There is a tendency of DDS and its providers to dismiss family members’ concerns about their loved one’s care as “overly dramatic” and to shut them out rather than investigate and address their allegations. This breakdown of the DDS-funded, provider-run residential system is especially alarming in the context of medical emergencies.
Fostering a DDS culture that acknowledges families as essential partners in collaboration is critical for improving outcomes for people with disabilities.
Families concerned they will be prevented from visiting loved ones at Christmas after having been barred on Thanksgiving
A nonprofit organization that was appointed as the guardian of at least two developmentally disabled individuals has imposed what appear to be illegal restrictions on visits to them from their families.
In each case, an employee of the corporate guardian, TLC Trust, Inc., appears to have been involved in preventing the families of Ryan Moran and Naomy Alicea from visiting them on Thanksgiving Day last month.
And in each case, Ryan’s and Naomy’s parents are concerned they will similarly be barred from visiting them in their Worcester-based group homes over the upcoming Christmas holidays.
The family members maintain in each case that the visitation restrictions have resulted from their complaints that their loved ones have been subjected to abuse or neglect in their provider-operated residences.
Naomy, 37, has an intellectual disability (ID) and cerebral palsy. Ryan, 29, has ID and is on the autism spectrum.
Hilda Natal, Ryan’s mother, said that the Department of Developmental Services (DDS) had Ryan placed in a group home run by Venture Community Services in 2020, when he was 24.
Naomy has been living in a separate group home in Worcester, which is operated by the Seven Hills Foundation. Both Venture and Seven Hills are DDS-funded residential providers.
Members of both families contend that their guardianships of their loved ones were removed for questionable reasons. DDS successfully petitioned in Worcester Probate Court to have TLC Trust appointed as the guardian of each individual instead.
It is unclear why TLC has been appointed as guardian of these clients. TLC’s website states that the organization primarily administers trusts with a minimum value of $100,000 for persons with developmental and other disabilities.
While the TLC website says the organization can also act as a corporate guardian for persons, the website further states that, “First priority for this (guardianship) service will be given to those individuals who have a trust relationship with the organization.” It does not appear that any such trust account with TLC exists in either Ryan’s or Naomy’s case.
We believe the visitation restrictions violate DDS regulations, which state that DDS clients have the “right to be visited and to visit others under circumstances that are conducive to friendships and relationships.” Also, the individual’s family members “shall be permitted to visit at all times, unless the individual objects…”
Visitation restrictions correlate with allegations of abuse or neglect
In both cases, the visitation restrictions appear to have followed from allegations by the families of neglect or abuse by the staff.
In each case, DDS and the corporate guardian appear to have blamed the families for causing problems such as allegedly causing agitation in their loved ones after their visits. But while clients may well become agitated, especially at the end of a visit, the cause of that agitation may actually be that the family member is leaving the client alone with the staff.
If there is neglect or abuse by the staff, that can be sufficient reason for a client to become agitated when the family member leaves.
Commissioner’s help sought in allowing visits
On November 25, I wrote to DDS Commissioner Sarah Peterson to urge that DDS allow Ryan’s family to visit him on Thanksgiving Day. Since then, we learned that a similar prohibition on visits was imposed on Naomy’s parents, and that TLC and its employee, Diane Parker, were involved in each case in imposing the restrictions.
As noted, neither family was allowed to visit on Thanksgiving. We are urging the Department to allow family visits during the Christmas and New Year’s holidays and to review the actions of TLC in restricting family visitation in each case.
Last week, Commissioner Peterson responded, thanking me for “reaching out with (my) concerns,” and saying she had “followed up with the local teams on the specifics of these cases. While I know you understand that I cannot comment on specific cases, please be assured that they are engaged and will follow up,” she wrote.
Peterson added that, “In terms of TLC Trust, Inc. serving as a guardian, I cannot speak to their requirements for taking private pay cases (which you identified from their website), but I can tell you that TLC Trust qualified through state procurement procedures to receive and accept appointments from DDS.”
Naomy’s case
Lizvette Rivera, Naomy’s mother, said she lost her guardianship of Naomy after a former family acquaintance made several accusations against Lizvette in 2018, which Lizvette and her other daughter, Catiria, claim were false.
DDS petitioned in Worcester Probate Court in 2018 to remove Lizvette as guardian and install TLC. Lizvette said her removal was based on the false accusations made against her, which were nevertheless presented as true in a Guardian ad Litem report to the Probate Court in 2019.
Lizvette and Catiria alleged numerous health scares at Naomy’s group home. They said that in one case, Naomy developed a urinary infection that required hospitalization because she was forced to shower by herself even though her family had repeatedly said she required support.
Naomy was subsequently prescribed medication that Lizvette and Catiria claim negatively altered her behavior. But when they questioned this, the residential staff imposed further visitation restrictions on them. They said they are frustrated by their inability to receive health information about Naomy from medical professionals, especially in light of her health complications.
Ryan’s case
Ryan’s mother and father, Hilda Natal and Jose Moran, said they have been barred from visiting him since early October because their visits were allegedly causing him emotional distress. As noted above, we strongly question whether it was the case that their visits could have caused that.
Jose said that on Thanksgiving day, he and Hilda tried to visit their son, but that the group home manager called Parker, the TLC Trust employee, who said visits were not being allowed by a DDS attorney. The house manager then threatened to call the police, and Hilda and Jose left.
Phone taken
Jose said that the group home staff also recently confiscated Ryan’s cell phone, with which he had been communicating with his parents on FaceTime. Jose said a staff member told him the phone was being kept in the group home office because the phone was not working. But Jose questions that because the phone is new. Without the cell phone, Ryan’s parents are only able to communicate with him via the group home’s landline phone in the office.
Hilda also said that when Ryan did have his phone, group home staff would stand outside his room, listening to his conversations. She said that in October, the house manager said Ryan would be required to leave his bedroom door open when he talked to his parents on his phone.
The DDS regulations cited above state that clients have the right to have reasonable access to a telephone other web-based communication, and the right “to make and receive confidential communications.” They also have the right “to keep and use personal possessions.”
Judge blames parents, but provides few details
In Ryan’s case, a probate court judge appears to have sided with DDS and TLC in finding that his parents’ visits to him were “problematic.” In a December 9, 2024, document titled, “Brief Findings and Rationale,” Worcester Probate Court Judge Roxann Tetreau stated that “visits with (Ryan’s) parents at the group home …would result in (Ryan) engaging in behaviors after they left.” As a result, the judge said, the group home and TLC restricted family visits.
Tetreau’s findings, however, provided no supporting details. The judge did state that: “It is again clear from the evidence that Jose and Hilda love their son…They do not, however, understand what (Ryan) needs…” The judge appears, however, to have accepted DDS’s and TLC’s claims about Ryan’s parents and to have disregarded the parents’ point of view.
Abuse and neglect of Ryan
There was also no mention in Tetreau’s findings of Hilda’s allegation that Ryan was repeatedly abused by staff in a day program job he had, starting in 2017. She said the abuse caused Ryan to have an anxiety crisis, and she then told him to stop working there. After that, she said, DDS petitioned in probate court to remove her as Ryan’s guardian. She said DDS made false statements in court about her and Ryan.
Neglect and restrictions on visits
Neglect and severe restrictions on family visitation imposed by group home providers seem to go together, and we have brought several of those cases to the attention of Commissioner Peterson in recent months.
When there is neglect and family members complain, the instinct of providers and DDS is often to deny families access to their loved ones in their residences. That way, the neglect itself does not have to be addressed.
We are asking that DDS investigate the allegations of abuse or neglect in each of these cases and to work with the families to find more suitable residential settings.
In the meantime, we are urging Commissioner Peterson to ensure that both of these families are allowed to visit their loved ones over the Christmas and New Year’s holidays.
Support COFAR this Holiday Season
Dear Members and Friends of COFAR,
Thank you for your dedication to the most vulnerable among us with intellectual and developmental disabilities. As we approach the holidays, we want to share our latest work and ask for your ongoing support.
We are continuing to advocate for families and guardians of clients in the Department of Developmental Services (DDS) system, as well as those caught up in the probate court system. We talk to people every day who feel overwhelmed by their treatment by DDS and the courts.
Whether it is attending court hearings as advocates on behalf of family members and guardians or enlisting the help of pro bono attorneys to assist them, we are committed to ensuring their voices are heard.
We are also deepening our outreach to legislators in opposition to bills that would replace guardianship with Supported Decision-Making (SDM), possibly marginalizing family members in the decisions most impacting their loved ones.
And we are working to enlist the aid of legislators and others in our effort to protect our state’s two remaining congregate care facilities—the Wrentham Developmental Center and the Hogan Regional Center. As you know, these centers are under siege by the administration and other proponents of privatized care who fail to recognize that the facilities provide a critical backstop for the care of persons around the state with the most profound levels of intellectual disability and the most serious medical issues.
We are further committed to the preservation and adequate funding of the state’s network of DDS-run group homes as an additional option for families and guardians seeking residential placements for their loved ones. After all, it is imperative that individuals and their families can choose the placements that best align with their needs.
Via our blog site, we provide unparalleled scrutiny of those and other issues, such as excessive compensation paid to provider executives and underpayment of direct-care staff.
Please consider a donation of whatever amount you can afford to help us continue advocating for you. You can contribute by going to our website at www.cofar.org and by clicking on the donate link. Or, you can send a check to our address (12 North Street, Leominster, MA 01453).
Thank you, and happy holidays!
Sincerely,
Thomas J. Frain, Esq.
President
As serious care issues remain under a new DDS-funded provider, a mother calls for systemic change
More than five years ago, Mary Phaneuf thought the serious neglect her foster son, Timothy Cheeks, had experienced in his group home in East Longmeadow was finally coming to an end.
In 2019, the Department of Developmental Services (DDS) took the rare step of terminating a contract with the Center for Human Development (CHD) to operate two residences, in one of which Tim was living. Among other problems, CHD, a DDS-funded corporate provider, had failed to take Tim to his doctor’s and dentist’s appointments for seven years even though Tim has a congenital heart defect.
COFAR’s blog posts in 2019 (here and here) concerning Mary’s allegations, and subsequent coverage by The Springfield Republican, led to a DDS investigation of CHD. The contract termination came after the investigation by DDS’s Bureau of Program Integrity found “potential systemic issues” of poor care throughout CHD’s residences.

Timothy Cheeks with his foster sisters, (from left) Nicole Phaneuf Sweeney, Lauren Phaneuf West, and Jessica Phaneuf Szczepanek.
DDS subsequently selected a new provider, the MHA (Mental Health Association), to replace CHD, and Tim was moved into an MHA home in 2019. Tim, 46, has an intellectual disability and Down Syndrome.
In September of this year, Mary got back in touch with us to let us know that many of the same issues that had existed under CHD began to reemerge under MHA.
In the early months, Tim’s care did improve significantly in the new residence. The new staff were communicative, attentive, and committed, Mary said. But as the COVID-19 crisis unfolded and management changes occurred, care started to slip, she said.
Nevertheless, Mary said she remains hopeful that the ongoing case will spark the systemic changes that she contends are necessary to permanently correct the problems.
“This is not to assign blame, but to advocate for change,” Mary wrote. “Many of the staff at MHA and DDS care deeply about the people they serve. The problem lies in a system that too often allows serious issues to repeat due to gaps in communication, training, and oversight.”
Since MHA has been in charge, the problems alleged by Mary include the following:
- In spring 2024, Tim’s Social Security benefits were terminated because of unreported income from his estranged biological father — a situation not caused by MHA, but requiring their timely response. However, the provider failed to meet the required federal timelines for an expedited appeal. As a result, Tim was without benefits for more than 18 months, leaving his personal funds depleted. His benefits were finally restored in October of this year.
- During the same period, Tim’s MassHealth insurance lapsed, interrupting access to medical and behavioral health services. The lapse occurred despite reminder emails from both the Behavioral Health Network (BHN), the provider of Tim’s counseling services, and DDS to MHA to renew Tim’s coverage. Coverage was only reinstated after family intervention.
- In September of this year, Mary discovered, for a second time, that Tim’s feet were red, swollen, and painful, with overgrown nails and large callouses that made it difficult for him to wear shoes. Although a podiatrist had recommended to MHA in February that Tim have follow-up visits every three months and receive prescribed twice-daily foot medication, he was not seen for seven months. Also, it appeared his medications were not being administered consistently.
- MHA staff initially falsely told Mary they stopped taking Tim to his podiatrist because the podiatrist had stopped accepting MassHealth. That claim was later refuted directly by the doctor’s office. This neglect violated Tim’s Individual Service Plan (ISP), which had specified podiatry care and weekly nursing visits for him, Mary said.
- In August 2024, over a year prior to her report in September of this year, Mary first reported to MHA and Tim’s DDS service coordinator that Tim’s feet were in bad shape. She showed them a photo of his feet with large callouses, toenails grown so long they curled over the top of his toes and a large fungal growth on the bottom of one foot. Mary said that after her 2024 report, DDS included Tim’s footcare in his ISP, and MHA committed to a weekly nurse visit to check his feet. “One year later it all fell apart,” Mary said.
- In October 2022, MHA staff gave another client’s high blood pressure and anti-psychotic medications to Tim. Although Mary was told Tim was “fine,” she arrived at the hospital to find him heavily sedated and disoriented. The Disabled Persons Protection Commission (DPPC) later substantiated the incident as abuse.
- In both 2024 and 2025, Tim’s behavioral counseling at Behavioral Health Network (BHN) was suspended due to missed appointments and unreturned calls to the group home. At one point, Mary was told Tim’s appointments were missed because his counselor was hospitalized — a statement BHN later confirmed was untrue. These missed sessions deeply affected Tim’s emotional stability and confidence, Mary said.
- In August 2024, Mary learned from Tim’s day program that MHA had failed to pay for or register him for day program activities for over a year, and that his funds for those activities had been depleted. Mary’s family covered the costs to prevent disruptions in his daily routine. MHA did fix that problem. But Mary said that if she hadn’t discovered it, MHA would have never known about it. “For a whole year those activities, so important for Tim’s quality of life, fell by the wayside,” she said.
Service coordinator supports allegations
In an email on September 3, Tim’s DDS service coordinator, suggested to Mary that she contact the DPPC regarding the alleged neglect of Tim’s feet and the lapse in his health insurance.
Having viewed the photos that Mary had sent him, the service coordinator wrote that an investigation by either the DPPC or DDS “will put a fire under the feet of MHA to ensure that they are following the podiatry/Dr’s orders, and making sure he gets the proper podiatry care. What you have sent in the pictures is unacceptable.” [Note: We are not publishing the photos due to their graphic nature.]
The service coordinator also stated, “Please don’t worry about anyone ‘getting in trouble’ at MHA. They need to do their jobs accordingly and also be truthful about the care of the people in their services.” He also referred to “Tim not having health insurance for 5 months,” saying, “That is simply not okay.”
Requests and promises of investigation of MHA
At our suggestion, Mary emailed the director of the DDS Bureau of Program Integrity on October 3 to let her know of the allegations involving MHA and to request another investigation. The Bureau had conducted the previous investigation of CHD in 2019. Mary also emailed the DDS Central West regional director and DDS Springfield area director, requesting an investigation.
Those officials responded to Mary the same day, saying they intended to look into the concerns she raised.
It is certainly both frustrating and devastating to Mary and her family to learn that even after an investigation that resulted in the termination of the provider that was neglecting Tim, similar problems have continued under the new organization selected as the replacement. It is a shame that such a vulnerable client has had to undergo this level of neglect twice, in two different residential settings.
All of this appears to show that DDS did not follow up to determine whether the problems identified by the 2019 investigation had been corrected. That investigation was, by all accounts, comprehensive. It is unfortunately more evidence that the group home system in Massachusetts is dysfunctional, and DDS does not have a handle on it.
Nevertheless, Mary said she believes that DDS and its providers are capable of providing good care and ensuring high staff morale and low staff turnover. She maintained that, “The ultimate goal is simple: to create a system where every person with a developmental disability receives consistent, compassionate, and competent care — and where families, providers, and the state work together to make that goal a reality.”
Mary noted that Tim loves music, his day program, and spending time with his family. “His laughter and resilience remind me why this work — ensuring quality care and dignity for people with disabilities — matters so deeply.” She said she remains hopeful that, “by working with MHA and DDS, we can make progress toward systemic improvement.”
We certainly hope that is the case.
COFAR appeals contradictory data from DDS on the population trend in state-operated group homes
Has the number of residents in the state-run network of group homes in Massachusetts for persons with intellectual and developmental disabilities (I/DD) been rising or falling?
We thought we had long known the answer to that question: The population or census of the group homes has been steadily falling. That conclusion was based on data provided to us in recent years by the Department of Developmental Services (DDS) in response to our periodic requests under the state’s Public Records Law.
But on September 18 of this year, DDS provided us with new data, in response to a new Public Records request, that contradict its previous numbers. That new data indicate that the census in the state-operated homes actually rose during the same fiscal years DDS had previously said it was falling – 2020 through 2023. Moreover, the new data show the census continued to rise until as recently as last month.
The problem is this discrepancy between the two sets of numbers from DDS leaves us uncertain what to believe. As a result, we have appealed to the state Public Records Division, asking them to order DDS to explain the discrepancy. So far, the Department has declined to do so.
The DDS state-operated group home network is far smaller than the privatized group home system, which is managed by DDS-funded corporate providers. DDS spends about $350 million a year in operating its state-run group homes, compared with more than $2 billion a year on the provider-operated homes.
But state-run services are just as important as provider-run services. We consider the state-run group homes and the Wrentham and Hogan congregate care centers to be the backbone of care in the DDS system. It has been our experience that staff in those state-run facilities are better paid and trained than staff in provider-run settings.
Yet, despite the fact that thousands of people with I/DD are waiting for residential placements and other services from DDS, the Department does not generally inform people seeking residential placements of the existence either of its network of state-run homes or of the Wrentham Developmental Center or the Hogan Regional Center. Instead, the Department directs those people to the much larger network of provider-run homes.
That’s another reason that a falling census in the state-operated group home system seems more likely to be the case than a rising census. In fact, it has long appeared that the administration does not view state-run residential services as viable options for waiting clients. DDS has, in our view, been letting the state-run system die by attrition.
Conflicting data regarding the census in state-operated group homes
So could it really be that the census has actually been rising in state-run group homes?
As noted, previous data from DDS showed a dropping census in the state-run group home system. During the period from Fiscal 2015 through 2024, that data showed the census had dropped from 1,206 residents to 986 – an 18.25% decrease.
Data provided by DDS on November 6, 2023, in response to a Public Records request, dovetailed with that previous data. The 2023 data showed the census dropping in the state-operated group homes by 2.9% between Fiscal 2020 and 2023.
However, in its latest response to our Public Records request on September 18, DDS provided data indicating, for the first time, that the census rose in the state-operated homes each year from Fiscal Year 2020 to 2023. The census in those years was now shown to have risen by 5.6%, rather than to have fallen by 2.9%, as DDS’s previous data had shown.
The census numbers provided by DDS on September 18 were on average 13% lower than the numbers that DDS had provided on November 6, 2023, for the same fiscal years.
The graph below shows the conflicting trend lines regarding the census based on those two contradictory sets of data from DDS.
Our appeal of the latest data response
Based on this discrepancy in the numbers between November 2023 and September 2025, we filed an appeal with the Public Records Division on September 24. We noted that the contradictory data made it impossible to determine which version represents DDS’s actual records.
We explained that the two data sets from DDS depict trends in opposite directions. We therefore asked the Public Records supervisor to direct DDS to clarify or reconcile its two sets of census data, or to explain in writing the reasons for the discrepancies so that the records provided would be comprehensible and complete.
On October 6, the Public Records supervisor denied our appeal, contending we hadn’t alleged a clear violation of the state’s Public Records Law (M.G. L. c. 66, § 10) by the Department.
On October 14, we asked the Public Records supervisor to reconsider her denial. We argued that under Section 10 of the Public Records Law, every state agency is required to respond to public records requests within 10 business days unless an extension or exemption applies. We noted that by producing two conflicting sets of census data for overlapping fiscal years—each purporting to respond fully to our records requests—DDS had failed to demonstrate that it had furnished the actual records it maintains as required by the law.
We further argued that under the Public Records law regulations [950 CMR 32.04(5)(b)], the agency “shall assist persons seeking public records to identify the records sought.” This duty necessarily includes responding in a way that allows the requester to understand what records are being produced. We noted that when an agency issues inconsistent responses for identical time periods, the requester cannot meaningfully identify the records received, frustrating the purpose of the regulation.
In addition, Section 10 of the Public Records statute authorizes the imposition of civil penalties when an agency has “failed to act in good faith in failing to furnish the requested record.” In issuing conflicting data for the same time frame without clarification, we maintained, DDS has not shown that it has acted in good faith or furnished a coherent version of the requested records.
Battle over records on vacancies in state-run group homes
Last year, we fought a similar battle with DDS to obtain records on the number of vacancies existing in the state-run group homes. DDS finally acknowledged it doesn’t track vacancies in the state-operated network.
We are hopeful that common sense will prevail in this case and that the Public Records supervisor will ultimately agree that the Public Records Law is meaningless if an agency can respond to requests by producing data that can’t be meaningfully interpreted.
In this case, the confusion is particularly frustrating. All we want to know is whether the census in the state-operated group homes is truly failing, as the data have clearly shown in the past, or whether that reported trend was incorrect.
So far, DDS, in their usual manner, has decided not to enlighten us on this important matter. We hope the Department will finally be ordered to do so.
Criminal charges against mother, who devoted herself to care of her disabled son, finally evaporate
Starting last year, Lisa Attenazio, the mother of a man with neurodevelopmental disorders, suddenly found herself fighting not only the state system of care in Massachusetts, but the court system as well.
For 27 years, Lisa maintains, things had gone smoothly for her and her son. But then her son’s girlfriend moved in with him, a state-funded attorney got involved, and things suddenly came crashing down. Lisa’s son has autism, aphasia, a disorder that impedes language comprehension and memory, and anxiety.
First, Lisa’s guardianship of her 27-year-old son was suspended, and a state-funded, temporary guardian was appointed in her place. This happened in August 2024, five months after her son’s girlfriend moved into his Winchester apartment with him and helped him retain the attorney, according to Lisa.
The attorney accused Lisa, without evidence, of “terrorizing her son” and petitioned in probate court to remove her as guardian and replace her with a guardian employed by the state.
Then in September 2024, Lisa was accused by the girlfriend of assaulting her and of violating a no-trespassing order that the girlfriend and Lisa’s son had taken out against her. And in June of this year, even Lisa’s son accused her of assault against him.
Lisa contends the criminal assault charges and the attorney’s allegations were manufactured against her out of whole cloth, and that she has never harmed anyone. She has many friends and supporters who say the same thing.
She claims her son was manipulated into pressing the assault charge against her and was also manipulated into frequently calling the police against her. She said he had never done that prior to his girlfriend moving in.
But Middlesex District Attorney Marian Ryan nevertheless pursued the felony assault charges against Lisa in both instances. Lisa’s son was prepared to testify against her in each case. (We are not disclosing either Lisa’s son’s name or his girlfriend’s name in this post.)
For a time, it appeared the probate court, the Winchester police, the District Attorney and even the Department of Developmental Services (DDS) and the appointed guardian had lined up together against Lisa to destroy her relationship with her son. “I was portrayed as someone whom I am not, and the lies, manipulation, brainwashing, and coercion have kept coming,” Lisa said.
Found not guilty
On Monday of last week (September 29), Lisa was found not guilty in Woburn District Court of the charge of assaulting her son. Judge Michael Callahan agreed that there was no evidence to indicate Lisa had assaulted him.
Roughly a month earlier (on August 19), the felony charge against Lisa of assaulting the girlfriend was dismissed after the girlfriend pleaded her Fifth Amendment right against self-incrimination.
But these two instances of vindication have come at a big cost, Lisa said. She is still fighting to get her guardianship back, and believes her son has regressed mentally and emotionally as the months of separation from her have gone by.
In August, Lisa even had to move out of her apartment, which was in the same building as her son’s apartment. She said she was living in constant fear of either her son or his girlfriend calling the police on her. Her court-appointed attorney in the assault cases against her, Paul Lawton, told her this was the saddest case he had ever seen.
By way of disclosure, I have acted on behalf of COFAR as an advocate for Lisa in probate court.
Mother supported son’s independence
Lisa had always gone the extra mile to be the best mother she could to her son.
In March, I first wrote about Lisa’s case, but used a pseudonym for her at the time. We are using her real name now because the issue has, in a key sense, shifted from her son to her.
Lisa contends her son is susceptible to manipulation by people who may not have his best interests at heart. She said this has been well-documented throughout his life.
As we originally reported, Lisa’s son wanted independence, and Lisa arranged with his clinicians to let him have his own apartment in Winchester in November 2023. At the advice of the clinicians with the Lurie Center for Autism, a division of Mass. General Hospital, Lisa herself moved into the same building, two floors below her son so she could be his “’safety net,’” in the words of the clinicians.
A few months later, in February 2024, Lisa’s son’s girlfriend moved in with him. Lisa said she believes her son’s girlfriend is not cognitively impaired although she is legally blind. Lisa said, however, that the girlfriend is able to see well enough to ride an E-bike and a motor scooter in the town of Winchester.
In March 2024, Lisa said, the girlfriend arranged for her son to be represented by a state-funded attorney. Lisa suddenly found herself accused by the attorney of being “emotionally unstable,” of “terrorizing” her son, and of refusing services for him. She said she was even accused at the time by the girlfriend of stealing her son’s car, when in fact, she owned the car.
Despite the fact that no questions had been raised about Lisa as a parent for the previous 27 years, a Middlesex County Probate court judge appointed Eva Toscano, who has worked for the Department of Mental Health, as temporary guardian for Lisa’s son in August 2024. Toscano had never known or met him. In court, DDS has supported the removal of Lisa as guardian.
Lisa maintains this all occurred because a guardian ad litem, appointed by the probate court judge, issued a report on the matter that was biased against Lisa. Our analysis of Lisa’s notes, which are based on the non-public GAL report, support her conclusion.
Lisa was then forbidden from talking to her son’s doctors, and even from entering her son’s apartment after her son and his girlfriend obtained a no-trespass order against her in September 2024. The Winchester Police Department subsequently filed a no-contact order with Lisa’s son. Lisa was also removed as her son’s representative payee for his Social Security payments.
Facing potentially years in prison
In September 2024, at the time of the issuance of the no-trespass order, Lisa was accused by the girlfriend of having assaulted her, which Lisa denied, and with violating the no-trespass order. Lisa now found herself facing criminal assault against a disabled person, a felony which carries up to a three-year prison sentence, and trespassing charges.
Lisa maintains that it was the girlfriend who assaulted her during a confrontation between the two of them in the son’s apartment. The Middlesex D.A., however, charged only Lisa in the matter. Lisa said the police ignored her when she suggested that the girlfriend be arrested.
A trial was set in Woburn District court for August 19 on the assault charge. However, just prior to the scheduled start of the trial, Lawton, Lisa’s attorney, asked the judge to appoint an on-duty criminal defense attorney to inform the girlfriend that if she did testify against Lisa, she could open herself up to prosecution for assault against Lisa.
That appointed attorney also advised the girlfriend that she could assert her Fifth Amendment right against self-incrimination. The girlfriend reportedly admitted to the attorney that she had been the aggressor and had struck Lisa first.
When the girlfriend was brought into the courtroom, the judge asked if she intended to plead the Fifth, and she said yes. At that point, the prosecutor said she had no basis for prosecuting the assault charge against Lisa, and asked that it be dismissed.
Second assault case also fizzles
On June 27, nine months after the first alleged assault incident, Lisa was accused by her son of assaulting him. Lisa was at that point facing two sets of assault charges as a result, and potentially five years in prison.
The police report regarding the second case involving Lisa’s son implied to us that her son was slightly injured by accident, through no fault of Lisa’s. On September 29, Woburn District Court Judge Callahan agreed. He found Lisa not guilty of the second assault charge.
Lisa maintains that her son was turned against her by his girlfriend in a way that doesn’t fit his personality. “He is not able to fully understand or comprehend or fully realize what’s going on but because he is rule governed,” Lisa said. “He will listen and do exactly what people tell him. Where is his voice in all this?”
Police reports disputed
Lisa was arrested on the first assault charge on September 17, 2024, after she allegedly violated the no-trespass order obtained by her son and entered his apartment. She maintains that her son obtained the no-trespass order at the urging of his girlfriend.
The Winchester Police report of the incident states that after being informed of the no-trespass order, Lisa went to her son’s apartment to collect some of her belongings there and to give her son her key fob for his apartment.
Lisa said she didn’t think the no-trespass order had yet gone into effect because her son led her into the apartment. She said she knocked on the door of the girlfriend’s bedroom to pick up some of the belongings, which she believed were there. The girlfriend claimed Lisa barged into the room.
According to the police report, the girlfriend said that after Lisa barged into the room, Lisa rushed at her and pulled her hair, struck her left brow with a closed fist, and then struck her in the left collarbone. The girlfriend also told police she “is almost fully blind and is legally disabled.”
Lisa told the police that when she entered the room, the girlfriend began to swear and scream at her and then shoved her and scratched her face and arms. Lisa claimed the girlfriend put her into a headlock, and she had to call her son to come and help her.
Although the two accounts were sharply conflicting, the police arrested only Lisa and booked her and fingerprinted her at the police station.
On August 19 of this year, the girlfriend reportedly admitted she struck Lisa first in the incident. As noted, the girlfriend subsequently asserted her Fifth Amendment right against self-incrimination, leading to the dismissal of the case.
Second assault case was an apparent accident
Lisa said the second case in which she allegedly assaulted her son occurred on June 27 when she tugged on his sleeve as he tried to leave her apartment following an argument about his use of the car. She said she was concerned that she remained responsible for paying for the insurance on the car even though she had been ordered to cease all contact with her son.
The Winchester police report of that incident states that Lisa “did assault and beat” her son – a charge that carries a potential sentence of 2 ½ years in prison. But that report described what largely appears to have been an accident.
According to the report, Lisa’s son called the police to the scene and told them he had attempted to leave Lisa’s apartment during the argument over the car, and that Lisa grabbed his t-shirt. The report stated that the son backed away, causing the shirt to tear. Then, it said, he lost his balance and fell backwards against the wall of the hallway and received a red mark or scrape on his back.
Lisa maintained that the police report was inaccurate in that respect. She said she grabbed the sleeve on his t-shirt and that after the sleeve started to tear, she let go, and her son tore the rest of his shirt. She said her son then turned and tripped and fell against the wall at her neighbor’s doorway, some 10 feet away.
The police report noted that Lisa told the police she was not being violent when she grabbed her son’s shirt, and that she would never hurt her son. She said she had offered to put aloe on her son’s back where he had scraped it. (Lisa said she actually did put aloe on his back.) The son later declined an offer by the police to be checked out at a hospital or to receive EMS assistance.
Lisa was nevertheless charged with assault and battery and was handcuffed, taken to the police station and kept in the lockup for seven hours before being released on $200 bail.
Lisa maintains that the Winchester police do not like her, possibly because they were frequently been called by her son or by his girlfriend to the apartment when there were disputes with Lisa.
Mother’s financial assistance continued
Despite the fact that the girlfriend and son had both filed the assault charges against Lisa, she said she continued to be expected, even by the state, to provide financial assistance to them.
For instance, Lisa said that on July 27, a month after filing the assault charge against her, her son left a note on her apartment door, asking if she was “still willing” to provide him with money to attend a summer camp in Maine for a week, and that she should leave it in an envelope in her car. The note ended, “Love and miss you xoxo.”
Lisa said the money would have been used by both her son and his girlfriend for spending-money at the camp in Maine. Even Toscano, the state-paid guardian, sent Lisa a message that day, also asking her to leave the money in her car for her son.
Lisa said she did not provide any money to her son for the summer camp, but the following day – July 28 – she received an alert from her son’s bank that he had incurred an overdraft in his checking account. So she did send $200 to his account to prevent other checks from bouncing.
Previously, on May 27, I emailed both the DDS attorney in Lisa’s probate court case, Barbara Green-Whitbeck, and her son’s court-appointed attorney, Mary Ann Remillard, expressing COFAR’s concern that Lisa was “expected and depended upon to act as both (her son’s) protector and financial provider even as her guardianship and authority as representative payee have been removed.”
At that time, I noted that Lisa’s son and his girlfriend had taken a trip to New Jersey and New York. While they were in New Jersey, they were unable to rent a car because they were using the son’s debit card and didn’t have sufficient funds on hand to pay a deposit required when debit cards are used. At that time, the son texted Lisa, to seek help. Lisa was forced to go to her bank to transfer $300 into her sons account in order to allow the car rental process to proceed.
What would have happened, I asked in my email to Green-Whitbeck and Remillard, if Lisa hadn’t been available? Her son and his girlfriend would have been stuck somewhere in New Jersey.
Neither Green-Whitbeck nor Remillard have responded to my email.
It remains puzzling to us that no one with official authority in this case appears to be able to see this matter from Lisa’s perspective.
Thankfully, both of the criminal cases against Lisa have now gone away — the first one when the girlfriend asserted her Fifth Amendment right, and the second when the judge found Lisa not guilty.
But Lisa’s life and her relationship with her son have been totally upended. We hope justice and common sense will prevail in this case and that Lisa will one day get her reputation and her son and guardianship back.

